The recent FDA 510(k) clearance granted to the Avatar Medical Vision platform represents a transformative shift in how surgical teams visualize complex anatomical structures by replacing traditional two-dimensional slices with immersive three-dimensional environments. This development marks the first time that regulatory bodies have authorized software specifically for use with glasses-free 3D medical displays, effectively lowering the barrier to entry for spatial computing in high-stakes clinical settings. By utilizing sophisticated algorithms to convert standard Computed Tomography and Magnetic Resonance data into interactive models, the technology allows physicians to perceive depth and spatial relationships that were previously obscured on flat screens. This advancement is not merely a visual upgrade but a fundamental change in the diagnostic pipeline, enabling a more intuitive grasp of patient-specific pathology while streamlining the preparation required for intricate procedures across various medical disciplines.
Bridging the Gap: The Technical Evolution of Surgical Visualization
The primary utility of this platform lies in its application across imaging-intensive specialties such as neurosurgery, oncology, and orthopedic surgery, where precision is measured in millimeters. Instead of mentally reconstructing a three-dimensional image from dozens of flat radiological slices, surgeons can now manipulate a digital twin of the patient’s anatomy to identify optimal entry points and avoid critical structures. This spatial awareness is particularly vital in oncology, where the proximity of a tumor to major blood vessels or nerves determines the feasibility of a resection. By providing a clear, depth-perceptive view, the system reduces the cognitive load on the surgical team, allowing them to focus on technical execution rather than spatial interpretation. The move away from cumbersome headsets toward glasses-free displays ensures that the entire operating room staff can share the same perspective without the physical discomfort or social isolation often associated with traditional virtual reality hardware.
Seamless integration into existing hospital infrastructure remains a cornerstone of the successful adoption of these advanced visualization tools within the modern healthcare environment. The platform connects directly with established Picture Archiving and Communication Systems, ensuring that high-resolution 3D models are generated almost instantly from existing patient records without requiring proprietary data formats. This compatibility minimizes the friction typically associated with implementing new software, allowing clinicians to access advanced annotation and analysis tools within their standard clinical workflow. Furthermore, the ability to utilize these tools across various hardware configurations—ranging from standard monitors to immersive spatial displays—provides hospitals with the flexibility to scale their technological investments according to specific departmental needs. By centralizing the visualization process, the software ensures that data consistency is maintained from the initial outpatient consultation through to the final intraoperative reference, fostering a unified surgical strategy.
Enhanced Communication: Transforming Patient Care and Strategic Outcomes
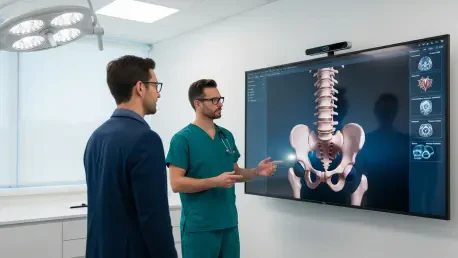
Beyond its technical merits in the operating room, the shift toward spatial imaging significantly alters the dynamics of the physician-patient relationship during the preoperative phase. Through a strategic partnership with Barco, the implementation of Eonis Vision displays allows doctors to present complex surgical plans in a format that is easily digestible for individuals without medical training. When patients can see their own anatomy in a vivid, three-dimensional space without the need for specialized eyewear, their understanding of the risks and benefits of a procedure increases substantially. This transparency fosters a higher degree of trust and encourages shared decision-making, which has been shown to improve patient satisfaction and recovery outcomes. The ability to visualize the intended surgical path helps demystify the process, reducing preoperative anxiety and ensuring that the patient is an informed participant in their own care. This collaborative approach turns the clinical encounter into an educational experience, bridging the gap between expert knowledge and patient understanding.
The transition from conventional 2D imaging to glasses-free 3D visualization represented a pivotal moment in medical history, fundamentally reshaping the landscape of surgical precision and patient engagement. Hospitals that adopted these integrated systems early observed a notable refinement in procedural efficiency and a reduction in planning time, proving that spatial computing was a necessity rather than a luxury. Moving forward, clinical administrators should prioritize the modernization of their display hardware to fully leverage these software advancements, ensuring that their facilities remain at the forefront of medical technology. It became clear that the successful implementation of such platforms required a multidisciplinary effort, involving radiologists, surgeons, and information technology specialists to maintain a seamless data flow. By investing in these intuitive interfaces, the medical community took a significant step toward a future where complex data was no longer a barrier to care but a clear roadmap for successful intervention. This evolution underscored the importance of accessibility in technological design for better health outcomes.