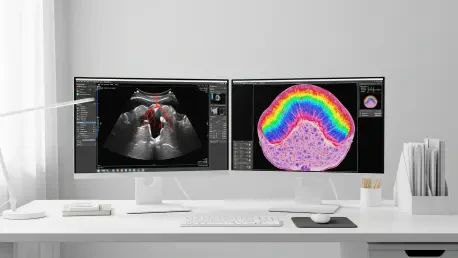
The historical reliance on computed tomography to merely map the structural integrity of coronary arteries has finally been superseded by a methodology capable of identifying cellular-level degradation. For decades, the primary objective of a cardiac CT scan was to identify stenoses or calcifications that might impede blood flow, acting essentially as a high-tech inspection of the heart’s plumbing. While effective for localized intervention, this anatomical focus often overlooked the physiological health of the myocardium itself. Recent breakthroughs spearheaded by researchers at Kumamoto University, notably Professors Yasuhiro Izumiya and Kenichi Tsujita, have introduced a delayed imaging phase that exposes what was once invisible to standard scanners. This evolution transforms the diagnostic process from a simple check for blockages into a comprehensive analysis of the heart muscle’s vitality, ensuring that silent damage no longer goes undetected in patients who appear healthy on traditional scans.
Modernizing Diagnostics: From Plumbing to Engine Health
Traditional cardiac imaging often prioritized the detection of obstructive coronary artery disease, neglecting the fact that the heart muscle itself can fail even when the supply lines are clear. This new diagnostic approach shifts the clinical focus from the “pipes” to the “engine,” recognizing that myocardial scarring and interstitial fibrosis are often the true drivers of adverse outcomes. Even in the absence of severe arterial narrowing, the heart muscle can exhibit subtle signs of distress that lead to diastolic dysfunction and eventually heart failure. By utilizing delayed-phase imaging, clinicians are now able to detect these hidden vulnerabilities during a standard examination. This capability provides an essential diagnostic layer, allowing for the identification of patients who are at risk despite having seemingly clear coronary arteries. The ability to visualize these structural shifts in real-time allows for a more nuanced understanding of cardiac pathology and long-term patient stability.
Beyond simple detection, this technological leap offers a prognostic window that was once the exclusive domain of Cardiac Magnetic Resonance Imaging (MRI), a resource-intensive modality. While MRI has long been considered the gold standard for tissue characterization, its application is frequently limited by high costs, long scan durations, and incompatibility with many implanted devices. The transition to enhanced CT protocols democratizes access to high-level cardiac diagnostics, making sophisticated tissue analysis available in a broader range of clinical settings. This shift is particularly vital for patients who require urgent assessment or those residing in areas where MRI availability is scarce. By integrating these advanced capabilities into the more common CT scanner, the medical community can identify early warning signs of heart failure much sooner than previously possible. This early detection is the cornerstone of preventative cardiology, enabling interventions that can significantly alter the trajectory of a patient’s disease before catastrophic events occur.
Diagnostic Pillars: Late Iodine Enhancement and Extracellular Volume
The technical core of this advancement rests on two sophisticated markers: Late Iodine Enhancement (LIE) and Extracellular Volume (ECV). Late Iodine Enhancement operates much like a spotlight, identifying specific zones of myocardial scarring that result from localized injuries or silent infarctions. When iodine contrast is administered, it lingers in areas where healthy muscle has been replaced by non-functional fibrotic tissue, allowing the scanner to capture a detailed map of permanent damage. This provides a clear visual record of the heart’s history, highlighting areas that are no longer contributing to the organ’s pumping efficiency. Identifying these focal points of damage is critical because they often serve as the substrate for dangerous arrhythmias and sudden cardiac events. Without the delayed phase of the CT scan, these scars would remain hidden, leaving clinicians with an incomplete picture of the actual risks facing the patient during their recovery and long-term management.
Complementing the localized data provided by LIE is the measurement of Extracellular Volume, which offers a broader perspective on the heart’s overall tissue health. ECV quantifies the space between heart muscle cells, serving as a surrogate marker for diffuse interstitial fibrosis, which is a widespread stiffening of the heart tissue. This condition is often a precursor to heart failure with preserved ejection fraction, a complex condition that has historically been difficult to diagnose in its early stages. By measuring the expansion of the extracellular matrix, doctors can identify the general wear and tear that affects the heart’s ability to relax and fill with blood properly. The synthesis of these two markers—one targeting specific scars and the other assessing general tissue stiffening—creates a comprehensive profile of myocardial integrity. This dual-layered approach ensures that both focal injuries and systemic degradation are accounted for, providing a level of diagnostic depth that traditional anatomical scans simply cannot achieve.
Clinical Implications: Validating Predictive Accuracy
The clinical validity of this enhanced imaging protocol was substantiated through an extensive observational study involving over 1,200 patients monitored over a significant period. The data revealed a striking correlation between myocardial abnormalities detected via delayed-phase CT and the occurrence of major adverse cardiac events. Specifically, patients who exhibited high readings in both Late Iodine Enhancement and Extracellular Volume faced a significantly elevated risk of unplanned hospitalizations and mortality. These findings emphasize that the condition of the heart muscle itself is a powerful, independent predictor of future health crises, often outweighing the predictive value of arterial blockages alone. This research effectively challenges the traditional reliance on coronary anatomy as the sole arbiter of cardiac risk. By proving that tissue health is a critical variable in the survival equation, the study provides a robust foundation for integrating delayed-phase imaging into the standard of care for cardiovascular patients worldwide.
This shift in diagnostic priority means that many patients who would have previously been cleared based on a standard CT scan can now be accurately identified as high-risk individuals. In many clinical scenarios, the degree of arterial stenosis does not tell the whole story, as patients with mild blockages can still suffer from extensive underlying myocardial decay. The ability to detect this “hidden” damage allows medical teams to move beyond reactive treatments and toward more proactive management strategies. By identifying these vulnerabilities early, healthcare providers can implement aggressive therapeutic interventions, such as specialized medication regimens or lifestyle modifications, tailored to the specific state of the patient’s heart muscle. This approach not only saves lives but also optimizes the use of healthcare resources by focusing intensive care on those who truly need it. The transition toward this more comprehensive model of assessment represents a significant milestone in the ongoing effort to reduce the global burden of heart disease.
Technological Progress: Enhancing Safety and Efficiency
The successful implementation of these advanced imaging techniques is largely due to significant improvements in CT hardware and post-processing software. Modern scanners now feature high-sensitivity detectors that can distinguish minute variations in iodine concentration within the cardiac tissue with unprecedented clarity. Additionally, sophisticated algorithms have been developed to reconstruct these images with high precision, ensuring that the data gathered is both accurate and reproducible across different clinical environments. These technical refinements have effectively transformed the CT scanner from a relatively simple anatomical imaging tool into a high-precision analytical instrument. This evolution allows for the seamless integration of delayed-phase imaging into existing clinical workflows without requiring specialized facilities. As these technologies continue to mature, the ability to extract detailed physiological information from a single, rapid scan will become increasingly central to the field of cardiovascular diagnostics.
Concerns regarding radiation exposure, which historically limited the use of multi-phase CT scans, have been effectively addressed through the development of low-dose protocols. By utilizing iterative reconstruction techniques and automated exposure controls, clinicians can now capture both the anatomical and myocardial data with minimal additional risk to the patient. This focus on safety ensures that the benefits of early disease detection far outweigh any potential downsides associated with the imaging process itself. Furthermore, the efficiency of the enhanced CT protocol significantly reduces the need for multiple diagnostic appointments, as blood flow and muscle health can be assessed in one session. This consolidation not only improves the patient experience by shortening the time to diagnosis but also lowers the overall cost of cardiac care for healthcare systems. By providing a faster, safer, and more affordable alternative to traditional multi-modality testing, the enhanced cardiac CT protocol is poised to become a staple of modern medical practice.
Clinical Implementation: Advancing Precision Cardiovascular Care
The integration of myocardial characterization into routine cardiac CT scans is a definitive step toward the realization of precision medicine within the cardiovascular field. Rather than applying generic treatment protocols based solely on the presence or absence of arterial blockages, physicians can now tailor their approach to the specific biological state of the heart. For instance, a patient identified with high ECV but no significant arterial narrowing might be treated more aggressively for underlying systemic conditions that contribute to fibrosis. This individualized approach ensures that therapies are targeted where they can be most effective, potentially reversing early-stage damage before it becomes permanent. As medical databases grow with this newly captured myocardial data, machine learning models will likely further refine these risk profiles, offering even more precise guidance for clinical decision-making. This proactive, data-driven strategy represents the future of cardiology, where prevention is prioritized over emergency intervention.
The medical community successfully established a new standard for heart health assessment by adopting these sophisticated imaging protocols in a widespread manner. Systems that prioritized the early adoption of delayed-phase CT observed a measurable improvement in patient risk stratification and a reduction in emergency department visits related to heart failure. Moving forward, it is essential for healthcare administrators to invest in the training and software updates necessary to support this diagnostic shift on a global scale. Collaborative efforts between researchers, clinicians, and technology developers have already paved the way for more resilient cardiovascular care frameworks that emphasize long-term tissue health. By focusing on the structural and functional integrity of the myocardium, modern medicine has secured a more comprehensive defense against the world’s leading cause of death. Future efforts must continue to refine these markers and expand their application to diverse patient populations, ensuring that the benefits of this diagnostic revolution are shared by all.