Ivan Kairatov stands at the forefront of a biological revolution where ancient clinical practices meet the cutting-edge precision of biopharma and systems neuroscience. As an expert in neuroimmunology, he has spent years decoding how physical interventions can be translated into molecular signals that the body uses to heal itself. The conversation today centers on a groundbreaking 2025 synthesis published in Acupuncture Research, which finally bridges the gap between traditional medicine and modern neurobiology. We explore the “mechanical-neural-immune” framework, a concept that moves beyond simple point-to-organ relationships toward a sophisticated understanding of how the brain and immune system communicate. Throughout our discussion, Kairatov unpacks how specific neural circuits—from the dorsal root ganglia to the vagus nerve—can be “programmed” through needle parameters to treat systemic inflammation and autoimmune conditions. This interview delves into the mechanics of sensory transduction, the role of the enteric nervous system in whole-body immunity, and the future of integrating artificial intelligence with bioelectronic medicine to create personalized, circuit-targeted therapies.
Traditional models often emphasize local stimulation, yet modern frameworks suggest a “mechanical-neural-immune” sequence. How do mechanosensitive receptors at the acupoint initiate these specific signals, and what role do the dorsal root ganglia play in relaying this information to the central nervous system?
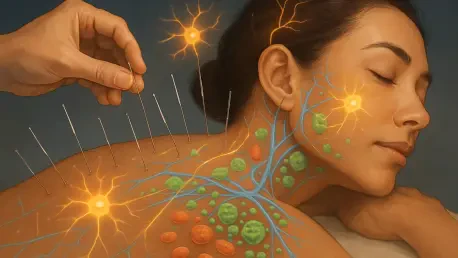
The shift from a local-only perspective to a “mechanical-neural-immune” sequence is truly the cornerstone of our modern understanding, as highlighted by the researchers from Fudan University and the China Academy of Chinese Medical Sciences. When a needle is inserted, it isn’t just piercing the skin; it is engaging in a complex dance with mechanosensitive receptors and the surrounding connective tissue, effectively transducing physical force into a sophisticated neural code. These signals are then swept up by specific sensory neurons located in the dorsal root and trigeminal ganglia, which act as the primary relay stations for the body’s internal surveillance system. I often visualize this as a high-speed data transfer where the physical “click” of the needle becomes a bio-electric message that travels directly to the spinal cord and brainstem. The dorsal root ganglia are essential here because they serve as the first point of integration, ensuring that the signal is robust enough to eventually engage higher-order autonomic outputs like the vagal or sympathetic pathways.
Acupuncture appears to induce local neurogenic inflammation and blood flow changes while simultaneously engaging the vagus nerve to suppress systemic inflammation. How do practitioners balance these immediate local responses with long-term autonomic shifts, and what metrics indicate these circuits have been successfully engaged?
Balancing the local “micro-storm” of neurogenic inflammation with the broad, calming effects of the vagus nerve is a delicate clinical art backed by rigorous systems biology. At the site of stimulation, we see a rapid remodeling of the immune microenvironment where mast cells and fibroblasts interact with sensory nerves to increase blood flow and release mediators. However, the real magic happens when this local activity triggers a vagus nerve-dependent anti-inflammatory pathway that reaches far beyond the needle to suppress the systemic release of inflammatory factors. Practitioners look for a “bidirectional” response, where the body’s autonomic nervous system dynamically adjusts immune cell activity based on the specific disease stage of the patient. Successfully engaging these circuits is often marked by shifts in heart rate variability or specific changes in immune cell distribution, proving that the intervention has moved from a local sensation to a coordinated, multi-organ immune modulation.
Factors like needle depth, frequency, and intensity dictate which specific neural circuits are activated. Can you provide a step-by-step breakdown of how adjusting these parameters changes the immune response, and what specific outcomes should be expected when targeting sympathetic versus parasympathetic pathways?
Adjusting stimulus parameters is essentially like tuning a radio to a specific frequency to find the right station; it determines whether you are speaking to the sympathetic or parasympathetic nervous system. For instance, a shallow needle depth with low-intensity stimulation might primarily engage the somatosensory-vagal reflex, which is excellent for triggering anti-inflammatory responses and restoring homeostasis. Conversely, increasing the intensity or frequency can flip the switch to the sympathetic nervous system, which might be necessary to mobilize immune defenses or adjust blood flow in a more aggressive, temporal manner. Step-by-step, the practitioner selects the “neural code” by varying the physical input, which then dictates which central integration center in the brainstem or hypothalamus is activated. The expected outcome of targeting the parasympathetic pathway is typically a systemic reduction in inflammation, whereas sympathetic targeting is often used for its more dynamic, context-dependent effects on immune cell behavior.
The enteric nervous system and gut barrier integrity are critical components of total-body immunity. In what ways does somatosensory stimulation influence the interaction between neuropeptides and gut microbiota, and what clinical anecdotes demonstrate this connection’s impact on managing chronic inflammatory or autoimmune disorders?
The 2025 review sheds significant light on how somatosensory stimulation reaches all the way to the gut, influencing the delicate interaction between the enteric nervous system and our resident microbiota. By activating specific neural circuits, acupuncture can strengthen the integrity of the gut barrier, effectively preventing the “leaking” of inflammatory triggers into the bloodstream. We are seeing that this process is mediated by the release of neuropeptides that communicate directly with gut bacteria, creating a feedback loop that helps regulate whole-body immunity. I have seen cases where patients with chronic inflammatory bowel issues or autoimmune flare-ups experience significant relief because the treatment essentially “re-educated” their gut-immune axis. It is a powerful reminder that the body is an interconnected network where a signal at a somatic acupoint can stabilize the microbial environment of the digestive tract.
Integrating acupuncture principles with bioelectronic medicine suggests a shift toward “programmable” neuromodulation. How might precision protocols using AI and multi-omics data transform traditional treatments, and what are the practical steps for incorporating these high-tech strategies into current clinical settings?
We are entering an era of “programmable” neuromodulation where we no longer rely on a one-size-fits-all approach but instead use data to drive precision. By integrating multi-omics data—which looks at everything from gene expression to metabolic profiles—with AI algorithms, we can predict exactly how a specific patient will respond to certain needle parameters. In a practical clinical setting, this would involve using bioelectronic devices that provide real-time feedback on neural circuit activation, allowing the clinician to adjust the “dose” of stimulation mid-session. This high-tech strategy transforms acupuncture from a traditional ritual into a data-driven medical intervention that can be aligned with emerging bioelectronic therapies. The goal is to move toward personalized, circuit-targeted therapies that focus on restoring long-term immune balance rather than just temporarily suppressing symptoms.
What is your forecast for acupuncture?
My forecast is that acupuncture will eventually lose its “alternative” label and become a primary pillar of bioelectronic and precision medicine. As we continue to decode the “mechanical stimulation-neural coding-immune response” framework, we will see the development of non-pharmacological protocols that are as rigorously tested and “programmable” as the latest biotech drugs. Within the next decade, I expect to see AI-driven acupuncture clinics where treatment is calibrated to the patient’s unique neural signatures, offering a powerful tool for managing the global rise in chronic inflammatory and autoimmune disorders. This evolution will bridge the gap between ancient holistic wisdom and 21st-century systems neuroscience, proving that the body’s own neural pathways are the most sophisticated pharmacy we have.