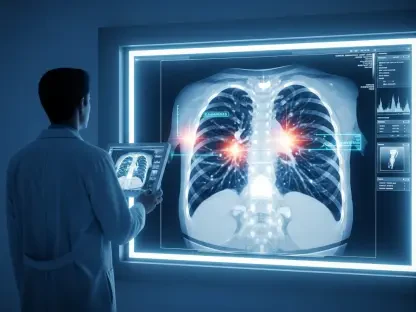
The persistent erosion of communal structures in the digital age has transformed what was once a private sorrow into a measurable physiological threat that rivals traditional oncological risks. While medical science has long focused on genetic predispositions and environmental toxins, a silent epidemic of social disconnection is now emerging as a critical factor in cancer development. This shift in perspective moves the conversation beyond simple feelings of sadness toward a rigorous assessment of how the absence of human interaction fundamentally alters bodily functions. By analyzing the intersection of social connectivity and cellular health, it becomes clear that the modern context of isolation is no longer just a psychological hurdle but a significant public health priority within the field of oncology.
The exploration into this phenomenon relies on sophisticated longitudinal findings that distinguish between physical solitude and the emotional state of being lonely. By examining biological pathways and gender-specific vulnerabilities, researchers are beginning to map the invisible threads that connect our social environments to our internal resilience. The strategic overview of these findings suggests that the structure of a person’s life—their actual, objective level of interaction with others—is a far more potent predictor of chronic illness than previously understood. This understanding forces a reassessment of how society approaches cancer prevention, shifting the focus from individual behavior to the strength of the community fabric.
The Divergence of Isolation and Loneliness in Health Data
Quantifying the Risk: Statistical Trends from the UK Biobank
Recent data derived from a massive longitudinal study of over 350,000 adults has provided a stark quantification of how objective social isolation contributes to cancer incidence. Over a tracking period of roughly 11.6 years, which allowed for the establishment of long-term oncological trends, researchers observed an 8% to 9% higher risk of cancer development linked directly to a lack of social ties. This statistical baseline serves as a foundation for understanding isolation not merely as a lifestyle choice but as a quantifiable health hazard. The sheer scale of the participant pool ensures that these findings are not merely coincidental but represent a significant shift in the epidemiological landscape of chronic disease.
An intriguing aspect of this data is the “loneliness paradox,” where the growth of objective social isolation as a risk factor contrasts sharply with subjective feelings of loneliness. While one might expect that feeling alone would be equally damaging, the research indicated that subjective loneliness did not independently increase cancer incidence when other variables were controlled. This suggests that the physical reality of being disconnected—the lack of regular visits, the absence of group participation, and living alone—exerts a unique pressure on the body that the psychological state of loneliness does not mirror. This distinction is vital for public health officials who must decide whether to target emotional support or physical community integration.
Real-World Implications and Site-Specific Findings
The manifestation of isolation in specific health outcomes reveals a troubling pattern of vulnerability, particularly regarding certain types of malignancies. In women, the lack of social connectivity showed a strong correlation with increased risks of breast, lung, and uterine cancers. These findings suggest that the hormonal and environmental stressors exacerbated by solitude may have a targeted impact on female physiology. In contrast, male demographics displayed a specific correlation between social withdrawal and an increased risk of bladder cancer. These site-specific findings indicate that the physiological fallout of isolation is not uniform but interacts with gender-specific biological systems in complex ways.
Moreover, the research identified a distinct “clustering” of unhealthy behaviors among those who are socially disconnected, which further compounds the primary risk of isolation. Individuals lacking robust social networks were more likely to engage in smoking, experience poor sleep quality, and maintain a high Body Mass Index. This behavior suggests that social ties often act as a regulatory mechanism, providing the accountability and support necessary to maintain healthy habits. When these ties are severed, the resulting behavioral shift creates a perfect storm of risk factors that accelerate the onset of disease. Consequently, isolation acts as both a direct biological stressor and an indirect gateway to other carcinogens.
Expert Perspectives on the Biological and Behavioral Bridge
Researchers specializing in mediation analysis have noted that the interaction between socioeconomic status and social connectivity creates a complex web of risk. Individuals with fewer financial resources often find themselves in environments that foster isolation, which then limits their access to the protective benefits of a community. This expert consensus suggests that social relationships should be classified as a “modifiable determinant of health,” deserving of the same clinical attention as diet or exercise. By treating social connectivity as a vital sign, healthcare providers can better identify patients who are at a higher risk of cellular mutation due to their environmental circumstances.
The biological link between isolation and cancer is increasingly found in inflammatory biomarkers such as C-reactive protein and neutrophil counts. Experts argue that chronic social stress keeps the body in a state of high alert, triggering a persistent inflammatory response that can damage DNA and impair the immune system’s ability to detect early-stage tumors. The significance of these markers lies in their ability to provide a visible, chemical signature of the invisible burden of solitude. This bridge between the social and the cellular demonstrates that the body interprets the lack of a “tribe” as a fundamental survival threat, leading to systemic changes that inadvertently favor the growth of cancerous cells.
Future Projections: Social Connectivity as Preventative Oncology
The future of healthcare is likely to move toward a model where social “prescriptions” are utilized alongside traditional medical treatments to mitigate the risk of chronic disease. In this evolving landscape, a physician might not only prescribe medication but also refer a patient to community-based interventions designed to repair social networks. As the global population continues to age, the challenges of maintaining connectivity will grow, potentially widening health disparities if left unaddressed. Developing systems that prioritize human interaction could become a cornerstone of preventative oncology, effectively treating the community as a component of the healthcare system.
However, the path forward is complicated by modern urban planning and digital shifts that often prioritize solitude and convenience over meaningful community engagement. If these trends continue to emphasize isolated living and virtual interaction over physical presence, the “social gradient” of health could become a permanent fixture of urban life. Mitigating this risk will require innovative digital tools that foster real-world connections and a reimagined approach to architecture and public spaces. The success of future public health strategies will depend on the ability to integrate social connectivity into the very fabric of daily life, ensuring that the biological need for companionship is met in an increasingly fragmented world.
Summary and Call to Action
The comprehensive analysis of social metrics and health outcomes demonstrated that the physical structure of a person’s social life remained a primary driver of cancer risk. The findings highlighted that while subjective emotional states were significant for mental well-being, the objective lack of human interaction was what truly catalyzed physiological decline. Public health authorities recognized that addressing the biological consequences of solitude required more than just psychological counseling; it demanded a fundamental restructuring of social support systems. Researchers established that the inflammatory responses triggered by isolation were measurable and preventable, provided that the underlying social disconnect was treated as a legitimate clinical concern.
Integrating social connectivity into the standard of care for preventative medicine emerged as an essential strategy for lowering global cancer rates. This required a shift toward viewing the patient not as an isolated biological unit, but as a member of a social ecosystem that either sustained or compromised their health. Stakeholders moved to implement integrated strategies that targeted the socioeconomic and behavioral clusters associated with withdrawal. By fostering environments that encouraged physical interaction and shared community responsibility, society took an active step in neutralizing one of the most subtle yet pervasive threats to human longevity. These integrated health strategies finally acknowledged that human connection is a fundamental biological necessity for survival.