The historical medical assumption that the thymus is merely a childhood organ that loses all relevance once an individual reaches maturity is being systematically dismantled by recent data suggesting it is actually a primary driver of lifelong systemic health. For decades, the scientific consensus focused on thymic involution—the process where lymphoid tissue is replaced by fat—as an inevitable and largely inconsequential part of aging. However, contemporary perspectives in regenerative medicine now identify the thymus as a cornerstone for systemic resilience, providing the necessary T-cell diversity to combat everything from seasonal viruses to burgeoning malignancies.
The shift from viewing the organ as a childhood vestige to an adult health indicator has significant implications for how clinicians approach geriatric health. When the thymus remains active, it continues to serve as a biological barometer for the body’s immune surveillance capabilities. Conversely, an accelerated decline in thymic integrity is often a precursor to broader physiological failure. Modern researchers are beginning to treat the state of this organ as a critical metric for assessing the true biological age of a patient, rather than relying solely on the date on a birth certificate.
Understanding the transition from active lymphoid tissue to fatty replacement is no longer just an academic exercise in histology. It has become a vital component of redefining immune aging, especially as the medical field moves toward proactive preservation rather than reactive treatment. This new understanding suggests that the ability of the adult body to maintain a functional thymus is one of the most significant factors in determining whether an individual will experience a healthy, disease-free lifespan or a period of extended morbidity.
Cutting-Edge Insights and Market Trends in Immune Assessment
AI-Driven Diagnostics and Deep Learning in Immunology
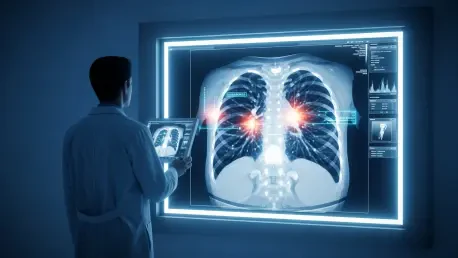
The revolution of imaging has arrived through the deployment of convolutional neural networks capable of analyzing computed tomography scans with a level of precision that exceeds human capability. These AI-driven tools can scrutinize the thoracic region to identify the subtle structural nuances of thymic tissue, distinguishing between healthy lymphoid density and non-functional fatty infiltration. By quantifying these features, developers have created a standardized Thymic Health Score, providing a clear, non-invasive metric for assessing immune potential in a clinical setting.
Self-supervised learning has further enhanced these diagnostic models by allowing algorithms to learn from massive, unlabeled datasets of medical imagery. This approach has enabled the identification of structural indicators of immune decline that were previously unknown to medical science. As these deep learning models become more sophisticated, they are being integrated directly into radiological software, offering real-time feedback to physicians regarding a patient’s long-term health trajectory.
Leveraging massive longitudinal data from established research cohorts like the National Lung Screening Trial and the Framingham Heart Study has been essential for predictive modeling. By cross-referencing thymic imaging data with decades of health outcomes, AI models can now predict a patient’s risk for specific diseases with high accuracy. This integration of historic data and modern technology is transforming the thymus from an overlooked anatomical feature into a central data point for personalized medical assessments.
Projecting the Impact of Immune Health on Global Life Expectancy
Quantifying the survival advantage associated with high thymic health scores has revealed that individuals with robust immune potential have a 50% reduction in all-cause mortality over a twelve-year period. This statistic is driving a major shift in the insurance and healthcare sectors, where “immune age” is becoming a key performance indicator for aging populations. The market for diagnostic tools that can measure this advantage is projected to grow significantly as more healthcare systems adopt longevity-focused protocols.
A forward-looking perspective on global life expectancy now centers on the transition from reactive care to proactive immune preservation. If healthcare providers can identify early signs of thymic decline, they can implement lifestyle or therapeutic interventions to slow the process of involution. This proactive stance is expected to add several years of quality life to the average adult, significantly altering the demographic landscape of developed nations.
The economic impact of this shift is equally profound, as increasing the period of “healthspan” reduces the duration of costly end-of-life care. By focusing on the thymus as a primary engine of longevity, the global medical market is moving toward a model where maintaining immune structural integrity is seen as the ultimate preventive measure. This trend is fostering a new generation of health technologies specifically designed to monitor and support the immune-longevity axis.
Navigating the Obstacles to Sustained Thymic Vitality
The challenge of inflammaging—a state of chronic, low-grade inflammation—remains one of the primary obstacles to maintaining thymic vitality. As the organ shrinks and produces fewer naive T-cells, the body becomes more prone to inflammatory responses, which in turn accelerates the degradation of the thymus itself. This cyclical process creates a difficult hurdle for clinicians, as breaking the cycle of inflammation requires more than just standard anti-inflammatory medications.
Lifestyle and environmental stressors, particularly smoking and poor metabolic health, are known to cause the accelerated degradation of thymic tissue. Research indicates that individuals with high levels of physiological stress or poor nutritional habits experience thymic involution much earlier than their healthier counterparts. Addressing these environmental factors is crucial for any strategy aimed at slowing the natural aging of the immune system and preserving the body’s defensive capabilities.
Furthermore, technological and observational gaps still exist, making it difficult to distinguish between simple correlation and true causation in some long-term health outcomes. While the link between thymic health and longevity is clear, the exact biological pathways that drive this connection are still being mapped. Strategies for preservation, such as potential therapeutic interventions and specific lifestyle modifications, must be refined through ongoing research to ensure they offer consistent benefits across diverse patient populations.
The Regulatory Landscape of Advanced Immune Diagnostics
Standardizing AI in clinical practice is currently a top priority for regulatory bodies, which must approve deep learning models before they can be used for formal diagnostic purposes. These organizations are working to establish benchmarks for accuracy and reliability to ensure that AI-generated thymic health scores are consistent across different imaging platforms. This oversight is vital for maintaining patient safety and ensuring that the data derived from these tools is clinically actionable.
Data privacy and security in longitudinal studies also represent a significant regulatory challenge, especially when managing sensitive health information across large-scale research cohorts. Protecting the anonymity of participants while allowing researchers to access the data necessary for predictive modeling requires a complex legal framework. As the use of AI in immunology grows, these security protocols must evolve to keep pace with new methods of data processing and storage.
Compliance with evolving standards for cardiovascular and oncological risk assessment is changing the way preventive care is delivered. Regulatory changes are increasingly encouraging the adoption of thymic screening in routine check-ups, especially for patients who are at high risk for age-related diseases. This systematic integration ensures that immune health assessment becomes a standard part of the medical landscape, moving from specialized research into the mainstream of clinical practice.
The Future of Longevity: Innovation and Disruptive Technologies
Regenerative therapies and thymic rejuvenation represent the next frontier of innovation, with scientists exploring bioengineering and tissue regeneration to restore organ function. The goal is to move beyond merely slowing decline and to actually rebuild the lymphoid tissue that has been lost to fatty replacement. If successful, these therapies could essentially “reset” a patient’s immune system, providing them with the defensive capabilities of a much younger individual.
Personalized immune monitoring is also on the rise, with biotech firms developing customized health plans based on individual thymic health profiles. This approach allows for a more granular level of care, where interventions are tailored to the specific rate of involution observed in a single patient. Such precision medicine is expected to disrupt the traditional healthcare model by focusing on the unique biological needs of the individual rather than broad population averages.
The global economic implications of these disruptive technologies are vast, as improved adult immunity could drastically reduce the burden of chronic disease on healthcare systems. Emerging market disruptors, including biotech firms focused specifically on the immune-longevity axis, are attracting significant investment. This influx of capital is accelerating the development of tools and treatments that could make the secret to a longer and healthier life accessible to a wider segment of the global population.
Summary of Findings and Strategic Recommendations
The scientific community successfully established the critical link between thymic health and resistance to major diseases, including cancer and cardiovascular conditions. Research proved that the structural integrity of this organ served as a foundational element of adult survival, influencing mortality rates and systemic resilience. These findings shifted the medical focus toward the preservation of immune function as a primary strategy for extending the human healthspan.
Healthcare providers identified the need to integrate thymic assessments into long-term patient wellness strategies to capture early signs of biological aging. This move required a new collaborative approach between radiologists, immunologists, and primary care physicians to interpret the data provided by AI-driven diagnostics. By adopting these tools, clinicians offered more accurate risk profiles and personalized intervention plans for their patients.
Investment and research opportunities focused on high-growth areas in immune-technology and geriatric medicine, specifically targeting the reversal of organ involution. Stakeholders recognized that the firms capable of developing effective rejuvenation therapies were positioned to lead the next era of medical innovation. These strategic investments were driven by the clear demand for technologies that supported the immune system’s role in lifelong health.
The medical landscape finally accepted the thymus as the critical missing piece in the puzzle of human longevity. Future protocols emphasized the maintenance of this organ as a non-negotiable component of preventive medicine, ensuring that the immune system remained a robust defense against the challenges of aging. These actionable steps paved the way for a future where immune structural health was prioritized as highly as any other vital sign.