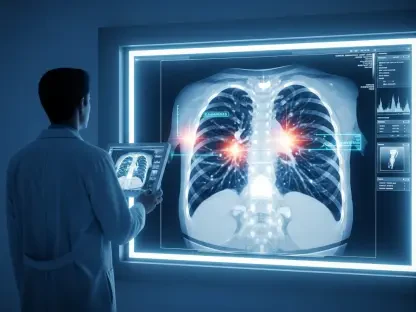
The clinical reality of a stroke is governed by a relentless biological countdown where approximately two million neurons perish during every single minute that blood flow remains obstructed to the brain. In the vast, windswept expanses of rural Oklahoma, this countdown has historically been a death sentence or a precursor to permanent disability due to the immense distances separating patients from specialized neurological expertise. While urban centers boast 24/7 access to stroke teams and advanced imaging, small-town residents often find themselves in “specialty care deserts” where the nearest neurologist might be hundreds of miles away. To combat this geographic inequity, Oklahoma has accelerated the deployment of telestroke technology, a sophisticated digital bridge that connects local emergency rooms with high-level specialists in real time. This initiative transforms the traditional healthcare model by bringing the expertise of a Tier 1 medical center directly to the patient’s bedside, regardless of their physical location within the state.
A compelling illustration of this technological intervention is found in the case of Eric Roath, a 44-year-old logger from Bethel whose physically demanding lifestyle seemed to offer a natural defense against cardiovascular events. When Roath suddenly experienced blurred vision and a loss of motor function on a September afternoon, his colleagues faced a grueling ninety-minute drive to reach McCurtain Memorial Hospital in Idabel. Under conventional circumstances, this delay would have likely pushed him past the critical therapeutic window, leaving him with profound long-term deficits. However, the hospital’s integration into the OU Health telestroke network changed the trajectory of his survival. Through a high-definition remote consultation, a neurologist located in Oklahoma City was able to evaluate Roath’s symptoms and authorize the immediate administration of thrombolytic medication. This timely intervention allowed him to achieve a near-total recovery, demonstrating that when digital connectivity is leveraged correctly, a patient’s zip code is no longer the primary determinant of their medical outcome.
Bridging the Rural Specialty Care Desert
Technology and Infrastructure in Rural Facilities
The geographic distribution of Oklahoma’s population presents a significant hurdle for healthcare equity, as nearly 40% of residents live in rural areas that lack the specialized staffing required for acute neurological care. To address this, the telestroke program has utilized substantial federal grants, including over $860,000 from the U.S. Department of Agriculture, to deploy advanced “telestroke carts” to dozens of critical access hospitals. These mobile units are not merely simple webcams; they are sophisticated medical devices equipped with high-resolution pan-tilt-zoom cameras and magnification capabilities that allow a remote neurologist to perform a detailed physical assessment. By viewing the patient’s pupils, testing motor responses, and communicating directly with on-site nurses, the specialist can make high-stakes decisions with the same level of confidence as if they were physically standing in the Idabel emergency room.
Implementing this high-tech solution requires far more than just unboxing equipment; it necessitates a comprehensive modernization of the physical and digital infrastructure within decades-old rural facilities. Many of these hospitals were constructed in the mid-20th century, long before the advent of high-speed fiber optics or integrated electronic health records. Upgrading these sites involves a massive overhaul of IT systems to ensure that massive neuroimaging files, such as CT scans, can be transmitted to specialists in seconds rather than minutes. This investment in the digital backbone of rural medicine is essential because even the most talented neurologist cannot provide a diagnosis if the hospital’s internet connection fails or if the imaging software is incompatible. These systemic upgrades represent a permanent improvement in the capabilities of rural hospitals, enabling them to participate in a broader range of telehealth services beyond just stroke care.
Clinical Workflow and the Critical Window
The gold standard for treating an ischemic stroke involves the administration of clot-busting drugs within a strict 4.5-hour window from the onset of symptoms, a timeframe that leaves no room for logistical inefficiency. The telestroke program optimizes this process through a highly synchronized clinical workflow that begins the moment a patient enters a rural emergency department. Local staff are trained to initiate immediate triage, which includes performing laboratory work and conducting a CT scan while simultaneously activating the remote neurologist. This “parallel processing” approach ensures that by the time the specialist logs into the secure platform, the necessary diagnostic data is already available for review. The neurologist can quickly rule out intracranial hemorrhages—where clot-busters would be fatal—and provide the local team with precise dosing instructions, effectively shrinking the time to treatment.
Beyond the immediate life-saving benefits, this collaborative model significantly alters the long-term management of stroke patients by reducing the frequency of unnecessary and expensive medical transfers. Historically, rural hospitals would automatically transfer any potential stroke patient to an urban center out of an abundance of caution, often via costly helicopter transport. Data from the current program indicates that approximately 50% of patients evaluated via telestroke can safely remain at their local facility for their post-acute care and recovery. This decentralization keeps patients close to their support networks, reduces the financial strain on families, and prevents urban tertiary care centers from being overwhelmed by cases that do not require specialized surgical intervention. By maintaining local care when appropriate, the program preserves the resources of the entire state healthcare system while improving the patient experience.
Strategic Funding and Regional Success Models
Financial Support and Institutional Buy-in
Sustaining and expanding a statewide telestroke network requires a diverse and reliable patchwork of financial resources, ranging from federal grants to state-level tobacco settlement endowments. Organizations like the Oklahoma Hospital Association utilize hundreds of thousands of dollars annually to help rural facilities achieve “acute stroke-ready” certifications, a designation that signals a hospital’s ability to provide high-quality initial care. These funds cover the costs of ongoing staff education, specialized equipment maintenance, and the rigorous data tracking required to maintain clinical standards. Without this continuous financial influx, the technological gap between urban and rural centers would inevitably widen again, as small-town hospitals often operate on razor-thin margins that cannot support the high costs of independent neurological consultations.
Successful integration of these tools also depends heavily on fostering a culture of partnership between local providers and remote specialists, rather than one of perceived replacement. For the program to work, local nurses and physicians must feel empowered by the technology, viewing the remote neurologist as an accessible colleague who enhances their own capabilities. This buy-in is achieved through intensive community outreach and on-site training sessions that demystify the technology and emphasize the collaborative nature of the care. Furthermore, public education campaigns focusing on the “FAST” acronym—Face drooping, Arm weakness, Speech difficulty, and Time to call 911—are critical to the program’s success. If the community does not recognize the signs of a stroke and seek immediate help, even the most advanced telestroke cart in the world remains useless, making public awareness an inseparable component of the technological solution.
Leveraging the Arkansas Model for Success
Oklahoma’s strategic direction has been heavily informed by the longstanding success of the Arkansas telestroke initiative, which has served as a national gold standard for rural health connectivity since its inception in 2008. By linking over 60 hospitals into a unified neurological network, Arkansas managed to bring 94% of its population within a 30-minute drive of a stroke-ready facility, a feat that Oklahoma is now striving to replicate. The Arkansas model proved that a centralized approach to telestroke could lead to massive cost savings—totaling nearly $60 million in a single year—by preventing long-term disability and reducing the need for nursing home placements. By following this regional blueprint, Oklahoma is adopting proven protocols for rapid notification and image sharing that have already demonstrated a significant downward trend in stroke-related mortality rates.
The ongoing evolution of the Oklahoma telestroke program suggests a future where the democratization of medical technology effectively eliminates the “Level 1” care disparity in small-town emergency rooms. As digital connectivity continues to improve and high-resolution imaging becomes the standard, the state is creating a comprehensive safety net that treats every resident with the same urgency, regardless of their proximity to a major metropolitan center. This shift in rural medicine ensures that the focus remains on the patient’s biological clock rather than the odometer on an ambulance. By transforming potential lifelong disabilities into stories of full recovery and return to work, the program proves that strategic investment in digital infrastructure is the most effective way to modernize healthcare for the 21st century. The success of this model offers a scalable template for addressing other specialty shortages, from cardiology to mental health, in rural America.
In light of the demonstrated success of the telestroke network, healthcare administrators and state policymakers should prioritize the expansion of this digital infrastructure to include other time-sensitive specialties. The immediate next step involves securing permanent reimbursement pathways for telehealth consultations to ensure the financial viability of these programs once initial grant funding is exhausted. Hospitals should continue to conduct regular mock-stroke drills to refine their coordination with remote specialists, ensuring that every second of the 4.5-hour window is utilized effectively. Furthermore, rural communities must maintain aggressive public awareness campaigns to ensure that residents can identify stroke symptoms early and utilize the high-tech resources now available at their local clinics. By entrenching these technological and educational protocols into the standard of care, Oklahoma has established a resilient framework that will continue to save lives and reduce the socioeconomic burden of neurological disease for years to come.