The conventional method of determining a pregnancy’s timeline has remained largely unchanged for nearly two centuries, relying on a mix of patient memory and rudimentary calculations that often miss the mark by weeks. For decades, pregnancy dating has functioned as an educated guess rather than a precise science, leaving expectant parents and healthcare providers to navigate a significant window of uncertainty. With the recent federal clearance of advanced artificial intelligence for delivery forecasting, the “due date” is shifting from a vague target toward a data-driven prediction, fundamentally changing the management of the 40-week journey. This transition marks the end of the “guess-timate” era, replaced by sophisticated algorithms that provide a clearer window into fetal development and maternal health.
As the medical community moves away from the reliance on a calendar and the date of a last menstrual period, the focus shifts to the integration of predictive analytics. This evolution is not merely about convenience; it is about providing a higher standard of care through objective data. By utilizing cloud-based software, clinicians can now offer a Predicted Delivery Date that reflects the biological reality of the individual pregnancy rather than a statistical average. This shift toward precision medicine represents a monumental step in obstetrics, offering a level of clarity that was previously impossible to achieve with traditional tools.
The End of the “Guess-timate”: Why Traditional Due Dates Are Evolving
The reliance on the Last Menstrual Period as a primary dating tool is a practice rooted in the 19th century, a time long before the advent of modern imaging. While this method provides a rough framework, it assumes a regular 28-day cycle and precise ovulation, variables that are frequently inconsistent among the general population. In a significant number of pregnancies, the lack of certainty regarding conception leads to an inherent margin of error that can complicate clinical decisions later in the third trimester. This ambiguity often results in unnecessary anxiety for families and a lack of precision in medical planning.
The transition toward AI-driven dating acknowledges that every pregnancy follows a unique trajectory. Instead of forcing a biological process into a rigid 280-day mold, the new technology analyzes specific data points to forecast when a baby is actually likely to arrive. This evolution represents a move toward personalized obstetrics, where the specific characteristics of the mother and fetus dictate the care plan. As these data-driven models become more integrated into routine prenatal visits, the concept of a single, static due date is being replaced by a dynamic, highly accurate prediction that can be refined over time.
The Limitations of Modern Gestational Forecasting
Traditional gestational forecasting faces significant hurdles, beginning with the human variable in ultrasound technology. Manual measurements, such as the crown-rump length, are subject to the expertise and technique of the individual technician. Small deviations in how a digital caliper is placed can lead to discrepancies in the estimated gestational age, creating a ripple effect that influences everything from screening schedules to induction dates. These human errors are often subtle, yet they contribute to a cumulative uncertainty that the medical field has long accepted as an unavoidable limitation of the craft.
Beyond technical variability, a significant portion of the population lives in “obstetric deserts,” where access to specialized maternal-fetal medicine is limited or non-existent. In these rural or underserved regions, the gap in specialized care means that irregular cycles or late prenatal care often go unmanaged by advanced diagnostics. The stakes are particularly high when considering preterm birth, which remains a leading cause of neonatal morbidity. Without accurate timing, the ability to administer critical interventions, such as corticosteroids for lung development, is compromised. This geographical and socioeconomic disparity highlights the urgent need for automated tools that can provide specialist-level accuracy regardless of the patient’s location.
From Linear Measurements to Holistic Analysis: How Delivery Date AI Works
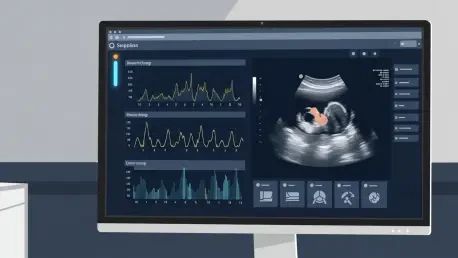
The technological leap in pregnancy dating is characterized by a shift from simple linear measurements to an “image-first” deep learning approach. Instead of relying solely on traditional rulers and calipers to measure fetal anatomy, advanced AI systems utilize massive datasets comprising millions of ultrasound images. These cloud-based neural networks are trained to identify subtle patterns and characteristics that the human eye might overlook. By analyzing the entire ultrasound scan—including fetal positioning and maternal markers—the software creates a holistic view of the pregnancy’s progression that far exceeds the capabilities of a manual assessment.
Furthermore, this technology is designed to be hardware-agnostic, allowing it to integrate seamlessly with existing ultrasound machines found in most clinics. This compatibility ensures that medical facilities do not need to invest in expensive new hardware to access advanced diagnostics. Once an image is captured and uploaded to the cloud, the AI processes the data and provides a Predicted Delivery Date in seconds. This real-time feedback loop allows physicians to discuss accurate results with patients during the exam, fostering a more collaborative and informed environment. The speed and accessibility of these systems are key factors in their rapid adoption across various healthcare settings.
Validating the Algorithm: Clinical Evidence and Expert Perspectives
The credibility of delivery forecasting AI is anchored in extensive clinical validation, most notably through the Perinatal Artificial Intelligence in Ultrasound study. This breakthrough research involved over 5,700 patients and demonstrated a high R² value of 0.92 for predictive accuracy. Such statistical strength indicates a very close correlation between the AI’s predictions and the actual delivery dates, providing a robust foundation for medical trust. This evidence-based approach is essential for shifting the paradigm of obstetric care, as it moves the technology from a conceptual tool to a validated medical device.
The significance of this technology is further underscored by its De Novo classification from the FDA, which establishes a legal and medical benchmark for AI as a “Software as a Medical Device.” Maternal-fetal medicine specialists view these systems as an “adjunctive tool” that enhances, rather than replaces, their clinical judgment. By providing an objective data point, the AI serves as a second set of eyes, particularly in high-risk scenarios where the timing of delivery is critical. This blend of human expertise and machine precision allows for a more nuanced conversation between doctors and parents, transforming how risks are assessed and managed in the delivery room.
Implementing AI-Driven Insights in Prenatal Care
Integrating AI-driven insights into standard prenatal care allows for the refinement of clinical intervention timelines. With a more accurate Predicted Delivery Date, providers can better time medical procedures such as inductions, specialized screenings, and the administration of steroids for high-risk patients. This precision ensures that interventions occur at the optimal biological window, maximizing their effectiveness and minimizing potential complications. The ability to tailor the prenatal schedule to the specific needs of the pregnancy represents a significant shift toward individualized care plans that prioritize the health of both the mother and the infant.
Moreover, the adoption of automated analysis helps to close the healthcare equity gap by bringing specialist-level accuracy to resource-constrained clinics. By providing a framework for integrating AI into standard obstetric workflows, the medical community can reduce the overall burden of preterm birth and improve outcomes across diverse populations. Providers can now rely on a standardized, data-driven approach that removes much of the guesswork associated with traditional dating. This systematic improvement in care delivery ensures that every patient, regardless of their background, has access to the most accurate information available regarding their baby’s arrival.
The medical landscape moved toward a future where the uncertainty of pregnancy dating was significantly diminished by the power of artificial intelligence. Clinicians adopted these advanced tools to replace outdated calculations, ensuring that every intervention was timed with unprecedented precision. The integration of cloud-based analysis provided a new standard for maternal-fetal medicine, bridging the gap between rural clinics and major medical centers. By prioritizing objective data over historical guesswork, the healthcare system established a more equitable and effective model for prenatal care. This technological shift fostered a safer environment for expectant families, as the focus remained on the health and stability of the next generation. Professionals across the country recognized that the evolution of gestational forecasting was a vital step in reducing the global impact of preterm birth and improving neonatal health outcomes.