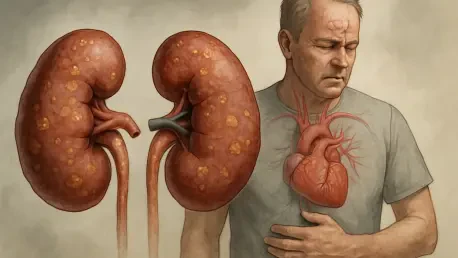
The silent progression of kidney disease has emerged as a formidable public health crisis in the United States, where nearly 15% of the adult population currently grapples with some form of renal impairment. These vital organs serve as the body’s primary filtration system, meticulously removing waste and excess fluids from the bloodstream to maintain a delicate internal balance. When this function is compromised, the body becomes susceptible to a cascade of life-threatening complications, ranging from sudden heart failure to debilitating strokes. The most insidious aspect of this condition is its lack of early warning signs, as roughly nine out of ten individuals remain entirely unaware of their declining organ health until the damage reaches an advanced, often irreversible stage. This high rate of undiagnosed cases has transformed the identification of new, modern risk factors into an urgent priority for medical researchers seeking to curb the growing prevalence of chronic illness.
Analyzing the Impact of Viral Infections
Understanding the Research Scope and Methodology
To quantify the long-term dangers posed by recent viral outbreaks, scientists at the Penn State College of Medicine conducted a rigorous analysis of a massive dataset encompassing over three million working-age adults. This comprehensive study utilized national insurance claims to track the health trajectories of individuals who contracted SARS-CoV-2 compared to those who experienced influenza or had no viral history. By focusing on a commercially insured population and excluding any participants with pre-existing renal issues, the research team ensured that the observed outcomes were directly attributable to the viral infections themselves rather than lingering baseline health problems. The methodology involved tracking these patients for a median of nearly a year, providing a sufficient window to observe how the body recovers—or fails to recover—from the systemic stress caused by the virus in a real-world setting.
The comparative nature of this research was essential for distinguishing between the general physiological strain of being sick and the specific, targeted damage caused by COVID-19. Researchers matched participants based on age, biological sex, and geographical region to account for environmental variables and the emergence of different viral variants over time. This structured approach allowed the team to isolate the unique “long-tail” effects of the virus, revealing that the damage to the renal system was not a temporary side effect of a high fever or dehydration, but rather a persistent pathological change. By establishing such a broad and controlled data pool, the study provides a high level of statistical confidence, suggesting that the history of a specific viral infection is a reliable predictor of future organ dysfunction. This level of detail is necessary for updating clinical protocols that have historically viewed respiratory viruses through a much narrower lens.
Disparity Between COVID-19 and Seasonal Illnesses
The statistical findings of the study revealed a stark and troubling disparity between the outcomes for COVID-19 survivors and those who had contracted influenza. While seasonal flu can certainly cause temporary stress on the body’s metabolic processes, the data indicated that COVID-19 survivors faced a 2.3-times higher risk of developing acute kidney injury, a condition characterized by a sudden loss of function that can occur within days. Even more concerning was the long-term outlook, as the risk of total kidney failure—which necessitates life-sustaining interventions like dialysis or an organ transplant—was nearly five times higher for those with a history of the virus. These figures demonstrate that the impact of SARS-CoV-2 on the kidneys is significantly more severe and sustained than the damage typically associated with other common respiratory infections that have circulated for decades.
Furthermore, the research highlighted that even those who did not require hospitalization during their initial infection were at an increased risk of developing chronic kidney disease later on. This suggests that the virus acts as a primary driver of renal dysfunction, potentially accelerating the aging process of the organs or triggering a low-level inflammatory response that persists long after the initial respiratory symptoms have cleared. The 1.4-times higher risk of chronic kidney disease observed in the study underscores the need for a fundamental shift in how the medical community views post-viral recovery. Instead of treating COVID-19 as a transient illness that ends once the cough subsides, clinicians must now recognize it as a systemic event with the potential to leave a lasting, detrimental footprint on the renal system, distinguishing it from the relatively predictable recovery path of the standard seasonal flu.
Biological Vulnerability and Modern Diagnostics
Why the Kidneys Are Uniquely at Risk
The biological explanation for why the kidneys are so frequently targeted by SARS-CoV-2 lies in the specific molecular architecture of renal tissues. These organs contain high concentrations of angiotensin-converting enzyme 2 (ACE2) receptors, which are the exact protein gateways the virus utilizes to enter and infect human cells. In essence, the kidney’s own cellular makeup acts as a “welcome mat,” allowing the virus to bypass traditional defenses and begin replicating directly within the organ’s delicate filtration units. This direct viral invasion can lead to localized inflammation, clotting in the small blood vessels of the kidney, and the destruction of the cells responsible for cleaning the blood. Unlike other viruses that primarily affect the lungs and only indirectly impact other organs through systemic stress, SARS-CoV-2 possesses the biological tools to launch a focused attack on the renal infrastructure itself.
Beyond the initial viral entry, the body’s own immune response can inadvertently contribute to long-term renal degeneration. When the immune system becomes overactive in its attempt to clear the virus, it can trigger a “cytokine storm” that causes widespread collateral damage to healthy tissues, with the highly vascularized kidneys being particularly susceptible. This combination of direct cellular infection and secondary immune-mediated injury creates a double-edged sword that can lead to both immediate, acute damage and a slow, progressive decline in function over several months. Because the kidneys have a limited capacity for self-repair compared to other organs like the liver, the damage sustained during a severe infection can set the stage for a permanent decline in health. Understanding these specific biological pathways is crucial for developing targeted therapies that can protect the organs during the acute phase of the illness.
Advancing Early Detection with Machine Learning
In light of these increased risks, the development of innovative machine learning models has become a vital component of modern renal care. Traditional risk-prediction tools for kidney disease often rely on dozens of variables, including body mass index, blood pressure, and complex genetic markers, which can make them cumbersome to use in a fast-paced clinical environment. However, the new models developed by the Penn State team have streamlined this process by focusing on just nine key variables, with a history of COVID-19 infection serving as one of the most powerful predictors of future decline. This technological advancement allows healthcare providers to identify high-risk individuals with greater precision and speed, often catching the early signs of organ stress before they manifest as physical symptoms or reach a critical stage that requires aggressive intervention.
The integration of artificial intelligence into the diagnostic process represents a significant shift toward proactive, data-driven medicine. By analyzing patterns within millions of patient records that would be impossible for a human to process, these machine learning tools can flag subtle trends in kidney function that might otherwise be overlooked during a routine checkup. This capability is especially important for a “silent” condition like kidney disease, where early intervention is the only way to prevent the eventual need for dialysis. As these models continue to be refined and integrated into electronic health records, they will empower physicians to provide more personalized care, moving away from a one-size-fits-all approach. This evolution in diagnostics ensures that the legacy of the pandemic is met with a equally sophisticated technological response, ultimately saving lives through earlier and more accurate screening.
Improving Long-Term Patient Care and Outcomes
The clinical implications of this research necessitate that a history of COVID-19 become a standard element of every patient’s medical screening and long-term health plan. Healthcare providers are now encouraged to implement more frequent monitoring of kidney function for survivors, particularly for those who already manage comorbidities such as hypertension or diabetes. Simple, low-cost tests like serum creatinine levels and urine albumin-to-creatinine ratios should be administered more regularly to ensure that any decline in filtration capacity is caught as early as possible. By shifting toward this proactive monitoring model, the medical community can mitigate the “long-tail” effects of the virus and provide patients with the lifestyle and pharmacological interventions needed to preserve their remaining organ function. This approach moves the focus from emergency treatment to sustainable, long-term health management.
Moving forward, the focus must remain on the integration of these findings into daily medical practice and public health policy. Educational initiatives aimed at both doctors and patients can help raise awareness about the link between viral history and renal health, encouraging individuals to advocate for their own screening even if they feel healthy. Future considerations should include the development of specialized “post-viral” clinics that offer comprehensive organ health assessments for those who experienced severe infections. As the global health landscape continues to evolve, the lessons learned from this study provide a clear roadmap for managing the intersection of infectious disease and chronic organ failure. By adopting a vigilant and technologically advanced strategy, the medical community can significantly improve the quality of life for millions of people who might otherwise fall victim to the silent progression of kidney disease in the coming years.