I’m thrilled to sit down with Ivan Kairatov, a renowned biopharma expert with extensive experience in research and development, as well as a deep understanding of technology and innovation in the industry. Today, we’re diving into the heartbreaking case of Leticia Paul, a young lawyer who tragically passed away due to anaphylactic shock following a CT scan with a contrast agent. Our conversation explores the medical details behind contrast agents, the nature of severe allergic reactions, and the critical safety measures needed in healthcare settings to prevent such incidents. We’ll also discuss broader implications for patient care and the importance of awareness around these rare but devastating risks.
Can you walk us through what happened to Leticia Paul during her visit to Alto Vale Regional Hospital on August 20, 2025?
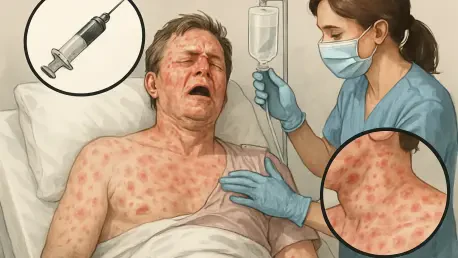
Thanks for having me, Chloe. The case of Leticia Paul is truly tragic. On that day, she underwent a routine CT scan at the hospital in Rio do Sul, Brazil, likely to investigate a history of kidney stones. During the procedure, a contrast agent was administered to improve the clarity of the images. Unfortunately, she experienced a severe allergic reaction to this substance, which quickly escalated into anaphylactic shock. Despite the hospital staff’s efforts to intervene, including intubation and other emergency measures, she passed away less than 24 hours later. It’s a stark reminder of how unpredictable and rapid these reactions can be.
What was the specific purpose of the CT scan for someone with her medical background?
Given her history of kidney stones, the CT scan was most likely ordered to assess the condition of her kidneys, check for any blockages, or identify new stones. CT scans are incredibly useful for visualizing the urinary tract, and contrast agents help highlight specific structures, making it easier to spot abnormalities. For Leticia, this would have been a standard diagnostic step, which makes the outcome all the more devastating.
Can you explain what a contrast agent is and why it’s so important in procedures like CT scans?
Absolutely. A contrast agent is a substance, often iodine-based for CT scans, that’s injected into the body to enhance the visibility of internal structures on imaging. It works by altering how X-rays pass through tissues, making blood vessels, organs, or abnormalities stand out more clearly. Without contrast, certain issues might be missed, so it’s a critical tool for accurate diagnosis in many cases, from detecting tumors to evaluating kidney function.
How common are side effects from these contrast agents, and what do they typically look like?
Most patients tolerate contrast agents without any major issues. Common side effects are usually mild, like a warm sensation, a metallic taste in the mouth, or slight nausea. However, allergic reactions, while rare, can occur. These can range from minor hives or itching to, in extreme cases like Leticia’s, full-blown anaphylaxis. The incidence of severe reactions is low—estimated at less than 1%—but when they happen, they demand immediate attention.
In simple terms, what is anaphylactic shock, and why is it so dangerous?
Anaphylactic shock is a life-threatening allergic reaction where the body’s immune system goes into overdrive in response to a trigger, like a contrast agent in this case. It releases a flood of chemicals that cause widespread inflammation, leading to symptoms like throat swelling, difficulty breathing, and a dangerous drop in blood pressure. It’s dangerous because it can progress within minutes, cutting off oxygen and potentially causing death if not treated immediately.
What are some of the warning signs that someone might be experiencing anaphylaxis?
The signs can come on very quickly and often include swelling, especially in the throat or face, which makes breathing hard. You might see hives or a rash, feel dizzy or faint due to dropping blood pressure, or experience a rapid heartbeat. Some people also feel a sense of doom or extreme anxiety. These symptoms are red flags that require urgent medical intervention, typically with epinephrine to reverse the reaction.
How fast do these symptoms usually show up after exposure to something like a contrast agent?
Typically, anaphylactic symptoms appear within seconds to minutes after exposure. With contrast agents, since they’re injected directly into the bloodstream, the reaction can be almost instantaneous. That’s why monitoring is so critical during and immediately after administration. In Leticia’s case, her condition deteriorated rapidly, which aligns with how fast anaphylaxis can strike.
What are some common triggers for anaphylactic shock, and where do contrast agents fit in?
Common triggers include foods like peanuts or shellfish, medications such as penicillin, insect stings, and latex. Contrast agents, particularly iodine-based ones used in imaging, are less common triggers but still significant, especially for patients with a history of allergies or prior reactions to similar substances. They fit into this category because they’re foreign to the body, and in rare cases, the immune system misidentifies them as a threat.
Is there a way to predict if someone might be at higher risk for a reaction to a contrast agent?
Predicting reactions can be challenging, but there are risk factors to consider. A history of allergic reactions, especially to iodine or previous contrast agents, raises the risk. Conditions like asthma or other allergies can also play a role. Doctors often ask about these before a scan, and in some cases, premedication with steroids or antihistamines is used to lower the risk. Unfortunately, without specific details on Leticia’s history beyond kidney stones, it’s hard to say if there were clear warning signs.
How is anaphylactic shock managed in a hospital setting when it happens?
The first line of treatment is epinephrine, usually given through an auto-injector or IV, to quickly reverse the reaction by opening airways and stabilizing blood pressure. Oxygen, IV fluids, and other medications like antihistamines or steroids may be used to support the patient. The hospital staff would also monitor vital signs closely and, if needed, provide advanced life support like intubation to help with breathing, which was attempted in Leticia’s case.
Despite these efforts, why do you think the hospital couldn’t save Leticia?
It’s heartbreaking, but even with the best interventions, anaphylaxis can sometimes be fatal if the reaction is too severe or if vital organs are deprived of oxygen for too long. In Leticia’s situation, despite intubation and emergency care, the rapid progression of her symptoms might have caused irreversible damage before treatment could fully take effect. Each case is unique, and sometimes the body’s response is just too overwhelming.
What safety protocols are usually in place when contrast agents are used in medical imaging?
Hospitals typically have strict protocols for using contrast agents. This includes taking a detailed patient history to check for allergies or past reactions, ensuring emergency equipment like epinephrine is readily available, and closely monitoring the patient during and after administration. Staff are trained to recognize and respond to allergic reactions swiftly. These measures aim to catch any issues early and intervene before they escalate.
Should hospitals be doing more in terms of screening or testing before using contrast agents?
There’s always room for improvement. While questionnaires about allergies are standard, they’re not foolproof since some patients may not know they’re at risk. Pre-testing for sensitivity to contrast agents isn’t routinely done because it’s not always predictive and can be impractical. However, for high-risk patients, alternative imaging methods without contrast or premedication protocols could be considered more often. Raising awareness among both staff and patients about potential risks is also key.
How often do severe reactions like Leticia’s happen with contrast agents, and what can be done to reduce these risks?
Severe reactions are quite rare. Studies suggest anaphylaxis from contrast agents occurs in about 0.01% to 0.04% of cases, though the exact numbers vary. To reduce risks, hospitals can ensure robust training for staff, maintain up-to-date emergency protocols, and invest in better patient education so individuals can report any unusual symptoms immediately. Technology, like improved contrast formulations with lower allergenicity, is also an area of ongoing research in biopharma.
Looking ahead, what is your forecast for improving safety around contrast agents in medical imaging?
I’m optimistic about the future. The biopharma industry is actively working on developing safer contrast agents with reduced risk of allergic reactions, potentially through non-iodine-based alternatives or agents tailored to individual patient profiles. Additionally, advancements in AI and predictive analytics could help identify at-risk patients before procedures. Combining these innovations with stricter safety guidelines and better training could significantly lower the chances of tragedies like Leticia’s. It’s about balancing diagnostic needs with patient safety, and I believe we’re moving in the right direction.