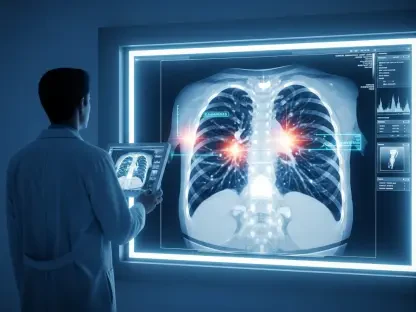
The realization that a medical diagnosis might arrive nearly two years too late has sparked a profound national debate regarding the efficacy of public health infrastructure within the Social Security Fund. A comprehensive audit of the National Center for Medical Imaging has revealed that patients requiring critical diagnostic support are currently facing wait times that can extend beyond six hundred days, effectively stalling essential treatments for life-threatening conditions. This delay is particularly devastating for those in the oncology department, where early detection serves as the primary line of defense against disease progression. The data suggests that the internal mechanisms designed to prioritize urgent cases have largely failed, leaving thousands of individuals in a state of medical uncertainty while their health continues to decline. As the public demands accountability, the focus has shifted from mere equipment shortages to a deeper investigation into the administrative bottlenecks that prevent timely access to care for citizens.
Administrative Dysfunction in Public Health Systems
Digital Disorganization: The SharePoint Failure
The audit specifically highlighted a reliance on a disorganized SharePoint platform rather than a consolidated medical registry, which has led to a complete breakdown in scheduling efficiency. This technical inadequacy means that medical staff cannot easily track patient priority levels or ensure that imaging is completed before crucial follow-up appointments with specialists. Instead of a streamlined workflow, the system operates in a fragmented manner where clinical urgency is frequently overlooked in favor of a chronological approach that does not account for the severity of a patient’s condition. Regulations requiring scans to be performed at least thirty days before a specialist review are routinely ignored, resulting in thousands of wasted appointments where physicians have no data to review. This logistical dysfunction has created a snowball effect, where the initial delay in scanning leads to a secondary delay in consultation, further complicating the patient journey.
Diagnostic Backlog: The Interpretation Crisis
Beyond the physical act of performing a scan, a massive backlog in the interpretation of existing studies has emerged as a significant barrier to effective healthcare delivery in the current 2026 landscape. Over 11,500 imaging studies currently remain unread, with some brain and neck scans waiting over 570 days for a formal report from a radiologist. This gap in the diagnostic process means that even when a patient successfully undergoes an MRI, the results are not immediately available to the treating physician, rendering the procedure useless in the short term. Consequently, medical teams are forced to make clinical decisions based on incomplete information or wait indefinitely for a finalized report, which keeps hospital beds occupied by patients who could otherwise be discharged. The audit notes that this failure to provide timely reports is not just an administrative oversight but a direct threat to the survival of patients whose conditions require rapid intervention.
Structural Solutions and Legal Obligations
Compliance Standards: Upholding Constitutional Rights
The investigative findings emphasize that these extensive delays represent a clear violation of constitutional mandates which dictate that health services must be delivered promptly and without interruption. Legal experts argue that the right to health is inextricably linked to the right to life, and a system that allows wait times to exceed eight hundred days fails its basic social contract with the citizenry. While the administration often cites a lack of resources as a primary cause for these failures, the oversight body has countered that poor management and a lack of accountability are the true culprits behind the current crisis. The audit suggests that the internal culture within the imaging center has prioritized administrative ease over clinical necessity, leading to a situation where even legal interventions from the courts have failed to secure timely care for some individuals. Addressing these issues requires a fundamental shift in how the institution perceives its duty to the public.
Strategic Reform: Implementing Modern Protocols
The oversight body concluded that a transition toward a risk-based scheduling approach was essential for restoring the integrity of the diagnostic system. It was recommended that the administration implement a modern, integrated registry that would automatically flag high-risk cases and ensure that imaging results were delivered within a timeframe that supported clinical decision-making. Strategic investments were prioritized not only in new machinery but also in the recruitment and retention of specialized radiologists who could manage the reporting workload more effectively. Furthermore, the report suggested that the immediate clearance of the existing backlog was a non-negotiable step toward preventing future bottlenecks and protecting patient safety. By establishing clear metrics for performance and holding department heads accountable for meeting them, the institution aimed to rebuild public trust and ensure that no patient would ever again be left in a diagnostic limbo for years.