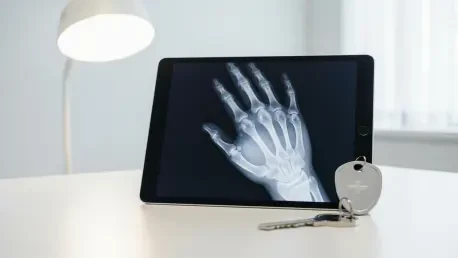
A seasoned radiologist stares at a chest X-ray, noting the crisp definition of the ribs and the clear expansion of the lungs, unaware that the patient on the screen does not actually exist. The gold standard of medical evidence—the diagnostic image—has officially entered the “uncanny valley,” a space where a synthetic fracture looks just as painful and authentic as a real one. Recent research published in Radiology has sent shockwaves through the healthcare community by demonstrating that generative AI can now create radiographs so convincing they bypass the critical eyes of veteran physicians. This is no longer a theoretical exercise in computer science; it is a direct challenge to the fundamental trust between a patient’s biology and the digital record used to treat it.
The implications of this shift are profound because the modern medical journey is almost entirely dictated by what a computer screen reveals. As healthcare systems move toward total digitization, the vulnerability of the Picture Archiving and Communication System (PACS) has become a primary concern for cybersecurity experts. The rise of sophisticated diffusion models means that “deepfake” medical images are no longer just low-resolution glitches, but high-fidelity fabrications capable of triggering unnecessary surgeries or masking life-threatening conditions. In an era where data-driven decisions dictate patient outcomes, the ability to indistinguishably alter a patient’s diagnostic history represents a systemic risk to insurance integrity, legal testimony, and clinical safety.
The Day the X-Ray Lied: A New Frontier in Medical Deception
The Radiological Society of North America (RSNA) facilitated an international, multi-institutional study to put both human intuition and algorithmic detection to the test. By analyzing how different demographics of experts and AI models handled synthetic data, the research uncovered startling gaps in our current defenses. This investigation was not limited to a single hospital; it involved 17 radiologists from six countries, representing a diverse range of experience from residency to 40-year veterans. Participants were presented with a dataset of 264 X-rays, including multimodal images generated by ChatGPT and chest radiographs produced by RoentGen, an open-source diffusion model.
This global cross-section provided a realistic look at how “generalist” and “specialist” eyes interpret synthetic data on a large scale. One of the most surprising findings was that seniority provided no protection against deception; veteran radiologists were just as likely to be fooled as their younger counterparts. While musculoskeletal (MSK) specialists showed a slight advantage due to their granular knowledge of structural anatomy, the average accuracy rate for detecting fakes—even after being warned of their existence—hovered at a mere 75%. This suggests that the visual cues we once relied on to identify authenticity are being successfully mimicked by generative algorithms.
Why the Integrity of the Digital Record Is Under Siege
The study also tested leading Large Language Models (LLMs) like GPT-4o and Gemini Pro to see if AI could catch its own handiwork. The results were inconsistent, with accuracy rates ranging from 57% to 89%. Interestingly, GPT-4o was the most successful at identifying images it helped create, yet it still failed to achieve a perfect score, proving that even the most advanced models cannot fully “unmask” the textures of modern deepfakes. This creates a paradox where the same technology used to advance diagnostic accuracy is simultaneously being used to undermine the veracity of the data.
Lead researcher Dr. Mickael Tordjman notes that the primary tell for a deepfake often isn’t a mistake, but rather a lack of human imperfection. He describes a “hyper-real” quality that serves as the main indicator for a forged image. Synthetic images often lack the “noise” of biological reality, appearing “too perfect” to be true. Experts identified several specific anomalies during the study, such as unnatural symmetry where lungs appeared as mirror images of one another—a phenomenon rarely seen in living patients—and linear rigidity where spines lacked the subtle physiological curves and wear-and-tear of a real human frame.
Breaking Down the RSNA Study: Humans vs. Machines
Beyond structural symmetry, the researchers observed that synthetic pathology often exists in a vacuum. In a real clinical setting, a fracture typically appears alongside secondary soft-tissue swelling or vascular irregularities that accompany trauma. AI-generated images, however, sometimes depict “clean” fractures that lack these biological consequences. This isolation of pathology is a hallmark of current generative models, which prioritize the visual representation of a condition over the complex, interconnected physiological response of a human body.
To prevent the erosion of trust in medical imaging, healthcare institutions must move beyond simple visual inspection and implement technical and educational safeguards. The most effective defense against deepfake injection is to secure the image at the point of origin through invisible watermarking and digital signatures. By embedding identity data directly into the image pixels and using cryptographic keys to link a specific X-ray machine to a file at the moment of capture, hospitals can ensure that any subsequent alteration is immediately detectable by the system.
Anatomical “Perfection” as a Red Flag: Insights from Dr. Mickael Tordjman
Radiologists must also be trained to recognize the specific “synthetic signature” of generative AI. The study advocates for the use of curated deepfake datasets in medical school curricula, shifting the focus from identifying disease to identifying the “hyper-smooth” textures and unnatural symmetries characteristic of AI-generated bone and tissue. This educational pivot would treat synthetic data detection as a new sub-specialty, essential for maintaining the chain of custody for diagnostic evidence.
The researchers concluded that the medical community needed to prepare for a future where 3D imaging, such as CT and MRI scans, would face similar synthetic threats. They suggested that developing specialized “adversarial” AI models—specifically designed to hunt for the fingerprints of generative algorithms—was a necessary step for hospital security. Furthermore, they emphasized that establishing standardized protocols for verifying image provenance became a mandatory requirement for legal and clinical certainty. By shifting from a culture of implicit trust to one of cryptographic verification, the healthcare industry aimed to protect the sanctity of the patient record against an increasingly invisible tide of digital fabrication.