The traditional image of a physician hunched over a keyboard, typing furiously while a patient describes their symptoms, is rapidly becoming a relic of a less efficient era. For decades, the administrative burden of clinical documentation has been the primary driver of physician burnout, with practitioners spending nearly two hours on paperwork for every hour of patient care. This friction between human connection and bureaucratic necessity has birthed the AI scribe, a sophisticated category of software designed to reclaim the exam room for the patient and the doctor.
The evolution of this technology has moved beyond simple voice-to-text dictation into the realm of ambient clinical intelligence. Unlike early speech recognition programs that required rigid verbal commands and manual editing, modern AI scribes utilize Large Language Models to interpret the nuances of natural conversation. These systems do not just transcribe; they filter out “noise”—such as small talk or environmental sounds—and extract medically relevant data to construct a coherent clinical narrative. This represents a fundamental shift from passive recording to active information synthesis.
Evolution and Fundamentals of AI Scribes
The journey of medical documentation has transitioned from handwritten charts to the digitized but clunky interfaces of early Electronic Health Records (EHR). In the current landscape, AI scribes act as a sophisticated bridge, leveraging Natural Language Processing to understand the hierarchical relationships within medical terminology. These tools are built upon neural networks that have been trained on vast datasets of medical literature and clinical encounters, allowing them to recognize complex diagnostic patterns and pharmacological interactions.
This technology has emerged as a direct response to the global healthcare staffing crisis. By automating the most labor-intensive part of the clinical workflow, these tools provide a scalable solution to administrative bloat. The core principle is “ambient” assistance, meaning the technology operates in the background, minimizing the cognitive load on the physician. This allows for a more natural, fluid exchange during the consultation, which has been shown to improve diagnostic accuracy by allowing doctors to observe physical cues they might otherwise miss while typing.
Core Components and Functional Architecture
Ambient Listening and Real-Time Summarization
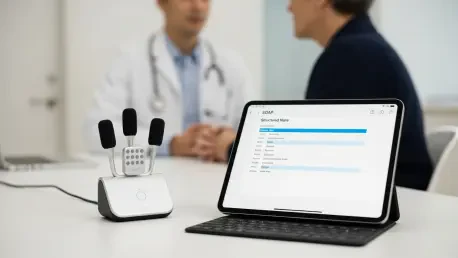
At the heart of the modern AI scribe is an ambient listening engine that employs far-field microphone arrays to capture high-fidelity audio from anywhere in the room. This hardware-software synergy allows the AI to distinguish between multiple speakers, such as the patient, their family members, and the clinician. Once the audio is captured, the summarization engine applies a clinical filter, categorizing the information into standardized formats like the SOAP (Subjective, Objective, Assessment, and Plan) note structure.
The performance of these systems is measured by their ability to maintain context over long durations. Advanced algorithms now possess the temporal awareness to link a patient’s mention of a symptom from three minutes ago to a specific medication discussed later in the session. This real-time processing ensures that the draft is ready for review almost immediately after the appointment ends, drastically reducing the “pajama time” doctors typically spend completing charts at home.
Integration With Electronic Health Records
A standalone AI tool is of little value if it creates another data silo; therefore, deep integration with existing EHR platforms is the true benchmark of a successful implementation. Modern scribes use Application Programming Interfaces (APIs) to push structured data directly into the correct fields of the patient’s digital file. This goes beyond simple text insertion; it includes the automatic population of ICD-10 codes for billing and the updating of medication lists, which reduces the potential for human transcription error.
This seamless data flow is what separates high-end professional tools from generic voice assistants. By syncing directly with the clinical schedule, the AI knows exactly which patient is being seen and can pull relevant historical data to provide context for the current summary. This interoperability is crucial for maintaining a longitudinal record of care, ensuring that every automated entry remains consistent with the patient’s broader medical history and treatment trajectory.
Current Trends in Medical Automation
The industry is currently witnessing a shift toward specialized AI models that are fine-tuned for specific medical disciplines. While a general-purpose AI might struggle with the specialized terminology of oncology or neurology, niche-specific scribes are being developed to understand the unique linguistic patterns of those fields. Moreover, there is a growing trend toward “proactive” AI, where the software does more than document; it suggests clinical guidelines or flags potential drug-drug interactions in real-time based on the conversation it is hearing.
Real-World Applications and Sector Impact
Beyond general practice, AI scribes are finding critical roles in high-pressure environments like Emergency Departments and intensive care units. In these settings, where every second counts, the ability to generate accurate records without manual input can be life-saving. Furthermore, the technology is making significant inroads in rural healthcare, where a single practitioner might oversee a massive patient load. By acting as a force multiplier, AI allows these providers to maintain high standards of documentation without sacrificing the number of patients they can serve.
Critical Challenges and Regulatory Obstacles
Despite the technological leaps, the “hallucination” problem remains a significant hurdle. AI models can occasionally invent details or misinterpret a patient’s denial of a symptom as an affirmation. Consequently, the clinician must remain the final arbiter of truth, reviewing every note for accuracy. Additionally, data privacy remains a contentious issue. While HIPAA compliance is a baseline, the use of de-identified clinical data to further train AI models raises ethical questions about patient ownership of their medical narratives and the transparency of third-party tech vendors.
Future Outlook and Policy Trajectory
The trajectory of AI clinical documentation is moving toward a total “invisible” infrastructure. Within the next few years, we can expect policy shifts that may mandate the use of such tools to ensure data standardized across entire health systems. Federal agencies are already exploring how AI-generated records can be used to streamline public health reporting and outbreak tracking. As these tools become more embedded in the legal and financial fabric of healthcare, their role will likely expand from simple secretaries to sophisticated clinical co-pilots.
Conclusion and Assessment
The adoption of AI scribes has fundamentally altered the clinical encounter, shifting the focus from the screen back to the patient. While the technology successfully reduced the administrative burden and improved the quality of life for many practitioners, it also introduced new responsibilities regarding data oversight and the verification of machine-generated content. The transition from manual to automated documentation was not merely a technical upgrade but a reimagining of medical labor. Moving forward, the focus must shift toward establishing robust ethical frameworks that govern data usage and developing more rigorous validation protocols to eliminate the risks of algorithmic bias. Healthcare organizations should prioritize the training of “AI-literate” clinicians who can effectively manage these tools as partners rather than just as passive users.