Ivan Kairatov is a distinguished biopharmaceutical expert with a formidable track record in research and development, specifically focusing on the intersection of technological innovation and clinical strategy. With years of experience navigating the complexities of large-scale vaccine trials and regulatory landscapes, Ivan has become a pivotal voice in discussing the evolution of infectious disease prevention. His insights are particularly vital as the industry grapples with shifting public health guidelines, the logistical hurdles of post-marketing commitments, and the economic pressures of a maturing vaccine market.
The following discussion explores the logistical and statistical consequences of halting massive clinical trials, the ethical tensions inherent in modern regulatory requirements, and the long-term impact of declining vaccine revenues on global pandemic preparedness.
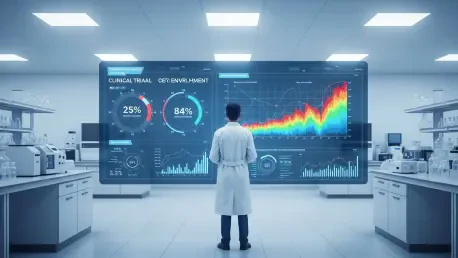
Enrollment in large-scale clinical trials for respiratory vaccines often slows during periods of low disease transmission. When a study requiring 25,500 participants is paused, how does that impact the statistical validity of data collected so far? Please detail the logistical steps for managing participants when a study is halted prematurely.
When you are aiming for a massive target like 25,500 participants and the recruitment engine stalls, the statistical power of the trial essentially evaporates. For a respiratory vaccine, you need a high volume of infection events to prove efficacy, and without those 25,500 data points during a “slow season,” the confidence intervals become too wide to draw any meaningful conclusions about whether the vaccine truly outperforms a placebo. Logistically, the wind-down is a complex, delicate operation that involves notifying every enrolled participant through their respective clinical sites to explain that the study is being suspended for reasons unrelated to safety. Investigators must meticulously document the “end-of-study” visits for those already enrolled, ensuring all adverse event reporting is up to date and that the database is locked to preserve the integrity of the partial data. It is a disheartening process for the teams involved because, despite the effort, the inability to generate relevant post-marketing data means the entire infrastructure built for the trial must be dismantled without reaching a definitive scientific finish line.
Federal regulators have recently moved toward requiring placebo-controlled arms for post-marketing studies even when authorized vaccines are available. What ethical dilemmas does this create for researchers? Please describe the specific trade-offs involved when recruiting healthy adults aged 50 to 64 under these stricter trial designs.
The shift toward requiring placebo-controlled arms in an environment where effective vaccines already exist is a profound departure from traditional trial ethics, creating a genuine “catch-22” for researchers. When we recruit healthy adults aged 50 to 64, we are asking a demographic that is still at some risk for severe outcomes to potentially receive a salt-water injection instead of a proven preventative measure. This creates a friction point where the scientific need for “gold standard” data clashes with the clinical duty to protect participants from a known pathogen. We see a significant trade-off in recruitment speed; many savvy patients in this age bracket are hesitant to enroll when they know they could simply go to a pharmacy and receive an authorized shot with a guaranteed active ingredient. Consequently, these stricter designs often lead to the very enrollment failures we are seeing now, as the “benefit-risk” proposition for the volunteer becomes much harder to justify.
National health guidelines now emphasize shared clinical decision-making and have narrowed recommendations for groups like healthy children and pregnant individuals. How does this shift toward individualized risk-benefit analysis change how manufacturers approach long-term data? Please explain the step-by-step impact this has on maintaining public health infrastructure.
The move toward shared clinical decision-making essentially shifts the burden of proof from broad population health benefits to highly specific, individualized outcomes. For manufacturers, this means we can no longer rely on massive, one-size-fits-all datasets; we have to pivot toward collecting more granular data that speaks to the specific risks and benefits for localized cohorts. This shift begins with a redesign of observational studies to track long-term safety in those specific groups—like healthy children—followed by a significant increase in the cost of medical affairs to communicate these nuances to healthcare providers. As the CDC narrows its recommendations, the public health infrastructure begins to fray because the predictable, high-volume demand that justifies maintaining massive manufacturing lines starts to disappear. Eventually, the step-by-step result is a more fragmented system where vaccine access is “severely limited” by policy, making it harder for the infrastructure to scale back up quickly if a new variant or a new pandemic emerges.
As revenue for established vaccine platforms declines, some developers are shifting resources toward oncology assets and reducing late-stage clinical investments. What specific financial metrics trigger such a strategic pivot? Please elaborate on how this shift might decrease the pharmaceutical industry’s readiness for future emerging infectious disease outbreaks.
The primary triggers for such a pivot are usually the “return on investment” (ROI) and the “net present value” (NPV) of the vaccine pipeline compared to high-growth areas like oncology. When we see a “waning access” to vaccines and a sharp decline in annual revenue—as we’ve observed with several major players recently—the board of directors often demands a reallocation of capital toward assets with higher pricing power and more predictable long-term margins. This “pull back” on late-stage vaccine trials is a dangerous trend because it leads to a “brain drain” of infectious disease experts and a decommissioning of specialized clinical trial networks. If we stop investing in the late-stage infrastructure for vaccines today, we won’t have the “warm” manufacturing sites or the ready-to-go enrollment centers needed to respond within the critical first 100 days of a future outbreak. Essentially, we are trading our global insurance policy against pandemics for the shorter-term profitability of cancer therapeutics.
What is your forecast for the future of COVID-19 immunization strategies?
I forecast that COVID-19 immunization will transition from a mass-market public health initiative into a specialized, seasonal boutique market focused almost exclusively on the high-risk and elderly populations. We will likely see the total volume of doses administered stabilize at a much lower level, perhaps only 20% to 30% of peak pandemic levels, as “shared clinical decision-making” becomes the dominant hurdle for the general population. This will lead to a consolidated market where only one or two manufacturers remain active, while others exit the space entirely to focus on more lucrative biologicals. Ultimately, the success of future strategies will depend on whether we can integrate COVID shots into a single, “multi-valent” seasonal respiratory vaccine that covers flu and RSV, simplifying the choice for the consumer and the provider alike.