The modern medical landscape is shifting toward a more holistic interpretation of preventative diagnostics, where a single scan can provide a comprehensive overview of a patient’s internal physiological state. Recent clinical observations indicate that low-dose computed tomography (LDCT) scans, originally designed to pinpoint early-stage pulmonary nodules, are increasingly serving as an early warning system for malignancies located outside the thoracic cavity. This evolution in diagnostic utility suggests that the value of routine screenings extends far beyond the specific organ they target, potentially saving lives by identifying hidden threats in the kidneys, liver, and lymphatic system. As clinicians refine their ability to interpret these incidental findings, the paradigm of lung cancer screening is being redefined to include a broader scope of oncological surveillance, ensuring that high-risk individuals receive a more thorough assessment of their overall health profile during their annual checkups.
Expanding the Scope of Diagnostic Imaging
Identifying Risks: Findings Beyond the Thoracic Cavity
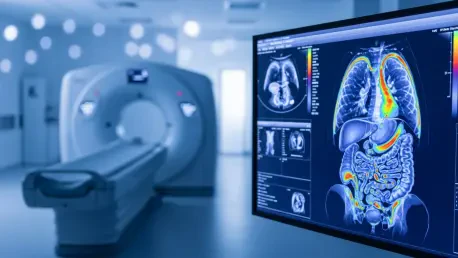
The primary function of a low-dose CT scan is to generate a series of detailed, three-dimensional images that allow radiologists to inspect the lung tissue for abnormalities. However, because the technology captures a broad section of the torso, the resulting imagery inadvertently includes a variety of other critical organs, such as the kidneys, adrenal glands, and the liver. These incidental findings, often referred to in the medical community as “incidentalomas,” have historically presented a complex challenge for healthcare providers who must distinguish between benign anomalies and life-threatening conditions. By expanding the analytical focus to include these extra-thoracic regions, medical professionals are now beginning to treat lung screenings as a multi-organ surveillance tool. This comprehensive approach ensures that asymptomatic patients who might be harborers of early-stage tumors in adjacent tissues are given a chance for early intervention before those conditions progress further.
Refining the diagnostic process for these unexpected discoveries is essential for reducing patient stress and improving overall clinical efficiency. For years, the presence of a non-pulmonary shadow on a scan could lead to confusion or delayed action, but the current research provides a structured evidence base to help clinicians prioritize certain findings over others. By categorizing these abnormalities based on their appearance and location, radiologists can now provide more definitive recommendations to primary care physicians. This systematic refinement means that a patient is less likely to undergo a battery of unnecessary tests for a harmless cyst, while simultaneously ensuring that a suspicious mass on the kidney is flagged for immediate follow-up. The goal is to maximize the diagnostic yield of every single scan, turning a routine procedure into a high-impact health assessment that covers multiple systems within the human body simultaneously.
Data Foundations: The National Lung Screening Trial
To establish a reliable framework for managing these incidental findings, researchers turned to one of the largest and most comprehensive datasets available in modern medicine. The National Lung Screening Trial (NLST) provided a massive repository of information, encompassing more than 26,000 participants and over 75,000 individual scans conducted over several rounds. This vast amount of data allowed the research team to track long-term health outcomes and correlate initial imaging results with eventual cancer diagnoses. By looking at such a large sample size, the study moved beyond anecdotal observations and toward a quantifiable model of risk assessment. This shift from guesswork to data-driven medicine is a cornerstone of modern oncology, providing a high level of statistical confidence that helps doctors make better decisions for their patients in the clinic every day throughout the current year.
The significance of this dataset is particularly high because the participants were primarily individuals with a significant history of tobacco use, a demographic that is already at an elevated risk for various types of cancer. While the screening was intended to monitor their lungs, the comprehensive nature of the NLST data revealed how frequently other malignancies appear in this population. By analyzing the outcomes of thousands of patients over several years, the researchers were able to identify specific patterns that link certain non-pulmonary abnormalities to future diagnoses. This evidence is vital for creating standardized protocols that can be used in hospitals across the country. It provides a roadmap for the medical community to follow, ensuring that every radiologist looks at the same indicators with the same level of scrutiny, regardless of whether they are working in a major urban research hospital or a small community clinic.
Statistical Insights and Cancer Types
Quantifying the Impact: Trends in Incidental Findings
The frequency of incidental findings during routine screenings is much higher than many patients or even some healthcare providers might initially suspect. According to the data, approximately one-third of all individuals undergoing a lung cancer screening will exhibit some form of abnormality that is completely unrelated to their pulmonary health. While most of these are benign, a specific subset of findings—roughly 3% of all screening rounds—is identified by radiologists as being highly suspicious for cancer. For the participants in the study, this meant that nearly 7% of the total pool encountered a finding that required serious medical attention over the course of their screening history. These statistics highlight the reality that a lung scan is often the first line of defense for a variety of health issues, providing a unique opportunity to catch problems that were not even being sought.
Most importantly, the research established a strong temporal link between these suspicious findings and the actual diagnosis of an extrapulmonary cancer. Patients who presented with these specific abnormalities were significantly more likely to receive a cancer diagnosis within just one year of the initial scan. this narrow window emphasizes the urgency of the findings and the effectiveness of the screening process as an early detection system. By quantifying these risks, the study provides a clear rationale for why physicians must pay close attention to every part of the image, not just the lungs. When a patient is told that an abnormality has been found, having these statistics allows the doctor to provide a more accurate prognosis and a clearer plan of action. This level of precision helps to ground the conversation in facts, reducing the ambiguity that often accompanies the discovery of an unexpected medical issue.
Specific Malignancies: Mapping Extrapulmonary Cancers
One of the most valuable aspects of the research is the identification of which specific types of cancer are most commonly detected through incidental findings on lung scans. The data showed a remarkably strong association between these screenings and the early detection of cancers within the urinary system, specifically those affecting the kidneys and the bladder. Because these organs are located near the bottom of the thoracic cavity, they are often partially or fully visible in a standard chest CT scan. Catching these cancers in their early stages, before symptoms like pain or blood in the urine appear, significantly improves the chances of successful treatment. This secondary benefit of lung screening serves as a powerful argument for the continued use of low-dose CT technology as a versatile tool for identifying aggressive tumors in the abdominal region.
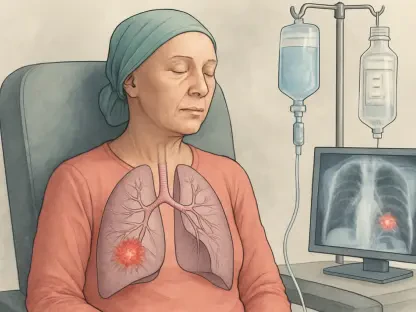
Beyond the urinary system, the scans also proved to be instrumental in flagging hematologic malignancies such as lymphoma and leukemia. These conditions often manifest as enlarged lymph nodes or abnormalities in the spleen, both of which can be clearly visualized during a thoracic imaging session. Furthermore, the scans provided early warnings for various abdominal pathologies, including issues with the liver and adrenal glands. By identifying these issues during a routine lung check, doctors are able to intervene months or even years earlier than they might have if they had waited for the patient to develop visible symptoms. This expanded diagnostic reach turns the lung cancer screening program into a broader surveillance network, catching a wide array of internal threats that might otherwise remain hidden until they reach a much more advanced and dangerous stage.
Refining Clinical Decision-Making
Balancing Act: Detection Versus Over-Treatment
A major challenge in the field of radiology involves the delicate balance between identifying potential threats and avoiding the pitfalls of over-diagnosis. While the goal is always to find cancer as early as possible, every incidental finding has the potential to trigger a series of follow-up tests, biopsies, and specialist consultations. This “cascade of care” can lead to significant patient anxiety, unnecessary physical discomfort, and a substantial financial burden on both the individual and the healthcare system. The researchers emphasize that the objective of their study is not to encourage more testing for every minor shadow, but rather to provide the data necessary to distinguish between high-risk abnormalities and those that can be safely ignored. This approach is essential for maintaining the integrity of screening programs and ensuring they remain a net benefit to public health.
By providing clearer guidance on which findings are truly indicative of cancer, the medical community can practice what is known as informed clinical management. This means that instead of reacting to every abnormality with an invasive procedure, doctors can use the study’s findings to categorize risks more accurately. For instance, if a specific type of adrenal mass has a very low correlation with malignancy according to the data, a physician might choose to simply monitor it with a follow-up scan in six months rather than ordering a biopsy immediately. This strategy reduces the number of “false positives” that lead to unnecessary surgery or stress. The focus remains on catching the 7% of cases that are actually dangerous while sparing the other 93% from the complications of over-medicalization, leading to a more streamlined and patient-centered approach to diagnostic imaging.
Strategic Management: Improving Overall Health Outcomes
The shift toward a more comprehensive interpretation of lung scans represents a strategic move in the management of long-term health risks for high-risk populations. Rather than viewing the discovery of a non-lung abnormality as a distraction or an error, modern medicine is beginning to see it as a vital piece of the patient’s health puzzle. This perspective is particularly important as the volume of people undergoing lung cancer screening continues to increase. As more individuals gain access to these preventative measures, the number of incidental findings will naturally grow, making it imperative to have a standardized system for managing them. This research provides the necessary framework to ensure that the healthcare system is not overwhelmed by the influx of data, but rather empowered by it to provide more accurate and timely care for every patient.
Furthermore, this evidence-based framework allows for a more productive conversation between doctors and patients regarding the potential outcomes of a screening session. When a patient understands that the scan is looking at more than just their lungs, they are better prepared for the possibility of an incidental finding. This transparency builds trust and ensures that the patient is an active participant in their own healthcare journey. By treating the lung scan as a broad health surveillance tool, the medical community can move away from a reactive model of care and toward a more proactive, preventative one. This strategic management of health risks ensures that resources are directed toward the most critical cases, ultimately improving survival rates and enhancing the quality of life for those at risk of developing various forms of cancer throughout the body.
The Future of Preventative Screening
Real-World Validation: Moving From Trials to Clinics
While the results derived from the National Lung Screening Trial were incredibly robust, the next phase of this medical evolution involved validating these findings in everyday community settings. Clinical trials are often conducted in highly controlled environments with the most advanced equipment and specialized radiologists, which may not always reflect the reality of a local hospital or a rural clinic. Researchers are currently working to ensure that the patterns of detection and the rates of incidental findings remain consistent across a diverse range of healthcare facilities. This involves analyzing data from various patient demographics and different types of imaging technology to confirm that the benefits of expanded screening are universal. Validating these findings in the real world is a crucial step in making these insights a standard part of medical practice everywhere.
This collaborative effort has brought together experts from some of the most prestigious institutions, including Duke Health and the National Cancer Institute, to ensure the findings are applicable on a broad scale. These organizations are focusing on how different imaging protocols might affect the visibility of extra-thoracic organs and how radiologists in different specialties interpret those images. By standardizing the way incidental findings are reported across all types of medical facilities, the healthcare industry can ensure a consistent level of care for all patients. This phase of the research also looks at how community doctors can best integrate these findings into their existing workflows without causing delays in treatment. The goal is to create a seamless transition from the research phase to the clinical application, ensuring that every patient who walks into a clinic for a lung scan receives the full benefit of this advanced diagnostic knowledge.
Conclusion: Establishing a New Standard of Care
The comprehensive analysis of lung cancer screening data successfully demonstrated that low-dose CT scans functioned as a powerful multi-organ surveillance tool. By documenting that nearly 7% of participants presented with findings that eventually led to an extrapulmonary cancer diagnosis, the research established a clear link between routine imaging and the early detection of kidney, bladder, and lymphatic malignancies. This evidence provided clinicians with a much-needed roadmap for navigating the complexities of incidental findings, allowing them to prioritize high-risk abnormalities while minimizing the risks associated with over-diagnosis. The study effectively shifted the diagnostic paradigm from a narrow focus on a single organ to a broader assessment of internal health, ensuring that patients received the most value possible from every screening session.
Moving forward, the medical community should adopt standardized reporting protocols that specifically account for these extra-thoracic observations to ensure no critical data is overlooked. Healthcare providers are encouraged to use the statistical models developed in this research to guide their follow-up recommendations, thereby reducing patient anxiety and the costs associated with unnecessary medical procedures. As screening technology continues to evolve and become more accessible, the integration of these findings into daily practice will be essential for maximizing the life-saving potential of preventative imaging. By remaining vigilant and data-driven, physicians can catch a wider array of cancers in their earliest, most treatable stages, ultimately leading to more efficient and compassionate patient care across the entire spectrum of oncological medicine.