Welcome to an insightful conversation with Dr. Ivan Kairatov, a distinguished neurosurgeon renowned for his expertise in rare skull base tumors and innovative surgical techniques. With a focus on sellar chondrosarcomas—a particularly uncommon and challenging condition—Dr. Kairatov has been at the forefront of advancing minimally invasive approaches like endonasal endoscopic surgery. Today, we dive into the complexities of diagnosing and treating these tumors, exploring their unique characteristics, the hurdles in clinical management, and the promise of modern surgical advancements. Join us as we uncover the intricacies of this rare disease and what it means for patients and clinicians alike.
Can you explain what sellar chondrosarcomas are and why they’re considered so rare compared to other skull base tumors?
Sellar chondrosarcomas are a type of malignant bone cancer that develops in the sellar region, which is at the base of the skull near the pituitary gland. They’re made up of cartilage-forming cells, which is unusual for this area, and they account for only about 0.2% of all skull tumors. Their rarity comes down to the specific conditions needed for this kind of tumor to form in such a confined and unique anatomical spot. Unlike more common skull base tumors, like meningiomas or pituitary adenomas, sellar chondrosarcomas originate from cartilage remnants or abnormal tissue development, which just doesn’t happen often in this region.
What are some of the typical symptoms patients with these tumors experience, and why do these particular signs show up?
Patients most commonly report blurred vision and headaches. About two-thirds of them experience vision issues because the tumor often presses on the optic nerves or chiasm, which are right nearby in the sellar area. Headaches, seen in about half the cases, likely stem from increased pressure inside the skull or irritation of surrounding structures. Additionally, a third of patients deal with endocrine disorders due to the tumor’s impact on the pituitary gland, which controls hormone production. These hormonal imbalances can sometimes improve after surgery if the pressure on the gland is relieved, though it’s not guaranteed.
Why is it so difficult to diagnose sellar chondrosarcomas before surgery, and what are they often mistaken for?
Diagnosing these tumors preoperatively is tough because their symptoms and imaging features overlap with more common sellar region issues. They’re frequently misidentified as chordomas, which are also rare but more familiar to clinicians, or as pituitary adenomas and craniopharyngiomas. Only one in a dozen cases might be correctly diagnosed before surgery. The similarity in clinical presentation—like vision loss or headaches—and the subtle differences on scans make it easy to assume a more typical diagnosis until you’re in the operating room or have pathology results.
How do imaging tools like MRI and CT scans help in identifying these tumors, and what specific features do clinicians look for?
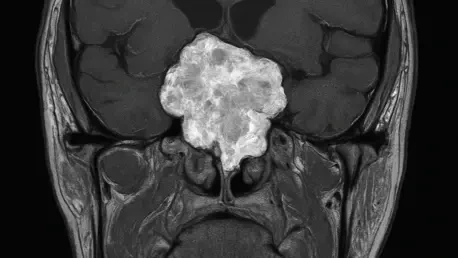
Imaging is critical for suspecting sellar chondrosarcomas, though it’s not foolproof. On an MRI, we look for heterogeneous enhancement, meaning the tumor shows uneven signal intensity, and a lack of diffusion restriction, which suggests free water movement within the tissue. These hints differentiate it from other masses. CT scans are great for showing bone destruction or how the tumor attaches to surrounding bony structures, which is a hallmark of chondrosarcomas since they often arise from cartilage near bone. Together, these tools help build a suspicion, but they can’t always confirm the diagnosis without a biopsy or surgery.
What has made endonasal endoscopic surgery a preferred approach over traditional transcranial methods for treating these tumors?
Endonasal endoscopic surgery has gained traction because it’s less invasive than opening the skull with transcranial approaches. By going through the nose with a thin tube equipped with a camera and tools, we can directly access the sellar region without disrupting brain tissue or leaving large scars. It reduces recovery time and lowers the risk of complications like brain swelling or infection. For patients, this means a quicker return to normal life, and for surgeons, it offers a clear, magnified view of the tumor, often allowing for precise removal despite the tight space.
Why is complete tumor removal achieved in only about half of the cases, and what challenges play into that?
Complete resection is tricky because of the tumor’s location and how it interacts with critical structures. These tumors often sit near the optic nerves, pituitary gland, and major blood vessels, so removing every bit can risk damaging those areas. In roughly half the cases, we have to leave some tumor behind to avoid harming the patient. Factors like the tumor’s size, how invasive it is, and whether it’s wrapped around delicate structures all influence whether total removal is possible. It’s a balance between being aggressive enough and protecting the patient’s quality of life.
How does incomplete tumor removal impact a patient’s long-term health, and what follow-up care is typically needed?
When we can’t remove the entire tumor, there’s a higher chance of recurrence, which can mean additional surgeries or treatments down the line. It also affects long-term health by potentially allowing continued pressure on nearby structures, leading to persistent symptoms like vision problems or hormonal issues. That’s why postoperative care often includes adjuvant radiotherapy to target any leftover tumor cells, especially if there’s clear residual disease. Regular follow-ups with imaging and clinical checks are crucial to catch any regrowth early and manage symptoms effectively.
Looking ahead, what is your forecast for the future of diagnosing and treating sellar chondrosarcomas?
I’m optimistic about where we’re headed. Advances in imaging technology, like more refined MRI sequences or even AI-driven analysis, could help us spot these tumors earlier and distinguish them from look-alikes with greater accuracy. On the treatment side, I expect endonasal endoscopic techniques to keep improving with better tools and navigation systems, making complete resections safer and more achievable. Additionally, targeted therapies or personalized approaches based on tumor biology might emerge as we learn more about the molecular makeup of chondrosarcomas. It’s a slow process given how rare these are, but each study and case brings us closer to better outcomes for patients.