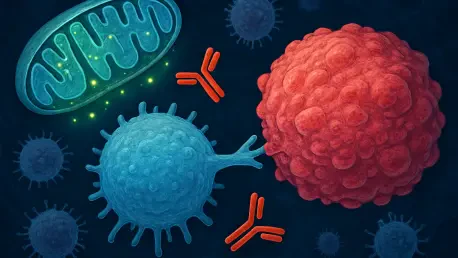
The human immune system operates like a sophisticated military intelligence network, yet even the most advanced radar systems can fail if their power supply is severed at the source. For years, the global struggle against malignancy focused primarily on unmasking cancer cells, assuming that once the disguise was gone, the body would naturally finish the job. However, clinicians often observed a perplexing silence from the dendritic cells, the essential gatekeepers tasked with identifying threats and sounding the alarm for T-cell activation. Recent scientific breakthroughs shifted this perspective, suggesting these sentinels were not merely deceived by the tumor’s camouflage; they were physically incapacitated by a catastrophic energy failure.
By reevaluating the immune response through the lens of cellular energy production, researchers began to realize that the secret to overcoming treatment-resistant tumors resided deep within the mitochondria. These tiny organelles, often relegated to the role of simple power plants in biology textbooks, proved to be the decisive factor in whether an immune cell remained active or fell into a state of metabolic exhaustion. This realization marked a pivotal shift in oncology, moving the conversation from purely genetic signaling to the physical fuel required to maintain an effective biological defense.
The Silent Power Crisis Within the Immune System
Dendritic cells serve as the primary sentinels of the human body, constantly surveying the biological landscape for signs of danger. When they encounter a malignant cell, their job is to process its specific markers and present them to the heavy artillery of the immune system, the T cells. However, in many advanced cancers, these sentinels appear to go dormant, allowing the tumor to expand without resistance. It was previously assumed that the tumor was simply invisible to the immune system, but closer inspection revealed that the dendritic cells were present but lacked the vitality to perform their duties.
This lack of vitality stems from a fundamental fuel shortage that occurs at the cellular level. When the mitochondria within these cells fail to function at peak capacity, the entire immune cascade grinds to a halt. The cells are no longer capable of synthesizing the necessary proteins or generating the electrical signals required to mobilize a defense. This energy crisis represents a silent bottleneck in immunotherapy, where the body possesses the correct blueprints for a counterattack but lacks the power to execute the construction.
The Bottleneck of Modern Oncology
Modern oncology relies heavily on immune checkpoint inhibitors, yet these groundbreaking drugs frequently hit a wall because they depend on an underlying immune architecture that is often fundamentally broken. In the suffocating confines of the tumor microenvironment, malignant cells act as resource gluttons, aggressively stripping the surrounding area of oxygen and glucose. This creates a metabolic desert where immune cells are forced to compete for survival, often losing the battle before they can ever mount a counteroffensive.
The result is a profound physiological disconnect where immunotherapy attempts to accelerate an immune system that essentially has an empty fuel tank. Understanding the metabolic health of dendritic cells has become a clinical necessity, as their failure to function properly prevents the entire cascade of anticancer responses from initiating. Addressing this energetic deficit emerged as the most promising path forward for the significant percentage of patients who remain non-responsive to existing standard-of-care treatments.
The OPA1-NRF1 Signaling Axis: Metabolic Shutdown
The collapse of dendritic cell function was eventually traced to a specific, tumor-driven reprogramming that effectively disabled the body’s primary alarm system. At the center of this metabolic sabotage lies a newly identified communication circuit involving the proteins OPA1 and NRF1, which manage mitochondrial structure and energy-related gene expression respectively. When dendritic cells venture into the hostile territory of a tumor, this OPA1-NRF1 axis is aggressively downregulated, serving as a biological kill switch that halts ATP production.
Faced with a terminal energy crisis, the dendritic cell prioritizes its own immediate survival, categorizing the high-energy task of immune activation as an unaffordable luxury. This strategic shutdown allows the tumor to continue its expansion undetected, effectively silencing the very cells meant to trigger its destruction. By identifying this precise molecular circuit, scientists gained a tangible target for interventions aimed at preventing the metabolic “off switch” from being flipped by the surrounding malignancy.
Evidence From the Front Lines: St. Jude Research
Rigorous investigations conducted at St. Jude Children’s Research Hospital provided the necessary empirical proof that restoring mitochondrial fitness could restart the immune engine. By using preclinical models, researchers demonstrated that engineering dendritic cells to maintain high levels of mitochondrial activity allowed them to bypass the suppressive effects of the tumor microenvironment. When these fortified cells were paired with conventional checkpoint inhibitors, the results surpassed expectations, as previously resistant tumors began to shrink under a rejuvenated immune assault.
Furthermore, the study highlighted a remarkable phenomenon known as durable immune memory, where the body retained the ability to recognize and destroy the same cancer long after the initial treatment. This suggested that a one-time metabolic intervention could potentially provide long-term protection against recurrence. The evidence from these trials underscored the reality that the success of immunotherapy depended less on the presence of the drug itself and more on the energetic readiness of the cells tasked with executing the command.
Strategies for Implementing Metabolic Immunotherapy
The transition toward metabolic immunotherapy required a fundamental pivot in how clinical frameworks and cell-based therapies were developed. Scientists focused on creating specific strategies to rewire the bioenergetics of the immune system, ensuring that the OPA1-NRF1 pathway remained active even under extreme physiological stress. This included the refinement of ex vivo priming techniques where a patient’s own immune cells were metabolically fortified in a controlled environment before being reintroduced to the body.
Pharmaceutical efforts also targeted the restoration of mitochondrial health, providing clinicians with a new set of tools to prevent cellular exhaustion in the field. By prioritizing the energetic requirements of the immune system alongside traditional signaling pathways, the medical community established a more resilient approach to cancer care. This holistic view of cellular fitness ensured that the body’s sentinels possessed the power necessary to lead a successful counterattack, ultimately transforming the landscape of oncology for patients facing the most difficult diagnoses.