The long-standing consensus that high-dose fish oil serves as a universal panacea for neurological health is currently undergoing a rigorous and necessary scientific recalibration. For years, the health and wellness industry has promoted omega-3 fatty acids as an essential defense against everything from cognitive decline to physical brain trauma. However, recent scientific inquiries are beginning to suggest that the traditional “one-size-fits-all” model of supplementation may be fundamentally flawed, particularly for those recovering from head injuries. Emerging data indicate that certain components of fish oil, specifically eicosapentaenoic acid (EPA), might inadvertently obstruct the brain’s natural ability to repair its vascular system following a traumatic event. This analysis explores why more of a supposedly beneficial substance is not always better and how the medical community is moving toward a more nuanced understanding of lipid-based recovery.
The Evolution of Omega-3s in Clinical Nutrition
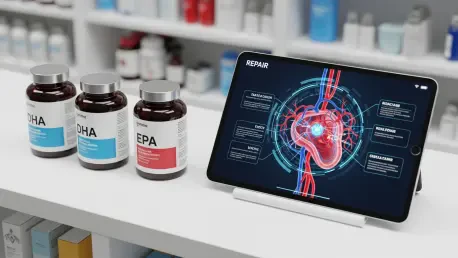
The trajectory of fish oil as a dietary staple began in the mid-20th century, largely driven by observational studies that linked high-fat fish consumption to improved cardiovascular outcomes. This early success catalyzed a massive market shift, transforming omega-3s from niche nutritional supplements into mainstream staples found in daily capsules and fortified food products. Within the field of neurology, the market solidified around two primary fatty acids: docosahexaenoic acid (DHA) and eicosapentaenoic acid (EPA). While DHA was quickly identified as a critical structural component of the brain, EPA gained popularity for its potent anti-inflammatory properties, leading many to believe that both were equally indispensable for neuroprotection.
This historical trust created a foundation where the complex interactions between these fats and injured neural tissue were often overlooked. By the turn of the decade, the industry had reached a point where chronic, high-dose supplementation was the standard recommendation for athletes, military personnel, and elderly populations. However, the lack of distinction between the long-term metabolic effects of EPA versus DHA left a significant gap in clinical understanding. As diagnostic tools have become more sophisticated, it has become clear that the “protective shield” promised by general omega-3 supplementation may have hidden costs, especially when the delicate blood vessels of the brain are tasked with self-repair after a concussion or repetitive impact.
Analyzing the Biological Mechanics of Recovery
The Metabolic Vulnerability of EPA Exposure
While DHA is known for its ability to integrate into the structural membranes of neurons, EPA follows a much more volatile and less predictable biological pathway. Recent research suggests that high concentrations of EPA can create a state of metabolic vulnerability within brain tissue. Unlike other fatty acids, EPA does not incorporate as readily into cell membranes; instead, its presence can shift how brain cells manage energy and respond to stress. In the context of traumatic brain injury (TBI), this shift appears to leave cerebrovascular tissue—the intricate network of blood vessels responsible for nourishing the brain—less capable of regaining stability.
Data from animal models indicate that subjects with high levels of EPA exposure demonstrate a significantly diminished capacity for vascular recovery following impact. This finding challenges the conventional wisdom that high-dose omega-3s are universally neuroprotective. Instead, the evidence points toward a scenario where the brain’s metabolic state is compromised by the very nutrients intended to save it. This vulnerability is not immediately apparent in a healthy brain, but it manifests as a “delayed deficit” once the tissue is forced to undergo the high-energy process of post-injury repair.
Disruptions in Vascular Scaffolding and Repair
The recovery process after a brain injury is fundamentally dependent on angiogenesis, which is the formation of new blood vessels from pre-existing ones. This process provides the necessary oxygen and nutrients for neural tissue to survive. Research involving human brain microvascular endothelial cells indicates that EPA may actively hinder this critical biological function. When these cells are exposed to high concentrations of EPA, the resulting angiogenic network is notably weaker and less organized compared to networks formed under the influence of DHA or standard conditions.
This disruption effectively suppresses the genetic instructions the brain requires to rebuild its vascular scaffolding. When the physical circulation system fails to reconstruct itself properly, the brain remains in a state of chronic instability and inflammation. This lack of robust vessel growth matches observed repair deficits in long-term clinical studies, reinforcing the idea that high-EPA environments prevent the brain from laying down the physical infrastructure needed for a full recovery. Consequently, the brain’s internal environment becomes a barrier to its own healing.
The Link Between Supplementation and Tau Protein Accumulation
One of the most concerning developments in this field is the observed accumulation of tau protein—a known marker of neurodegenerative disease—around the blood vessels of the cortex in subjects with high fish oil intake and repetitive head impacts. This perivascular tauopathy is a hallmark of conditions like Chronic Traumatic Encephalopathy (CTE). The data suggest that chronic EPA supplementation may inadvertently accelerate cognitive decline by interfering with the brain’s glymphatic system, which is responsible for clearing toxic proteins from neural tissue.
By disrupting the stability of the blood vessels, EPA appears to “trap” these harmful proteins in the perivascular space. This transcriptional reprogramming of the cortex suggests that the timing and duration of supplementation are just as critical as the specific fatty acids used. Instead of acting as a shield, the long-term presence of high-dose EPA might create a biological environment where the brain is more susceptible to the cumulative damage of repetitive impacts, leading to earlier onset of neurological symptoms.
Future Horizons: The Shift Toward Precision Nutrition
As the market moves forward, the field of clinical nutrition is pivoting away from generic, mass-market recommendations and toward a model of precision nutrition. From 2026 to 2030, it is anticipated that future guidelines for brain injury recovery will become highly personalized. These guidelines will likely account for an individual’s specific metabolic state, age, and professional history of head trauma. Technological shifts in diagnostic testing are already allowing clinicians to measure fatty acid transport mechanisms in real-time, helping to identify which patients are metabolically suited for specific omega-3 profiles and which should avoid high-EPA formulations altogether.
The regulatory landscape is also expected to change, with supplement manufacturers potentially facing new requirements for labeling and dosage recommendations. We may see a shift where high-EPA products are specifically cautioned against for populations at high risk of head injury, such as contact sports athletes or active-duty soldiers. The goal of this new era is to ensure that nutritional interventions align with the specific physiological needs of the brain at various stages of health and injury, rather than applying a broad, unrefined approach to lipid management.
Strategic Recommendations for Brain Health Management
For consumers and healthcare professionals, the current evidence necessitates a move toward more calculated strategies regarding fish oil use. It is now essential to distinguish between DHA-dominant and EPA-dominant supplements, especially for individuals whose occupations involve physical risk. Prioritizing whole-food sources of omega-3s—such as wild-caught fish—provides a more balanced profile of fatty acids that the body is evolved to process, rather than isolated and potentially disruptive high-dose extracts.
Furthermore, patients recovering from traumatic brain injuries should prioritize consultation with neurologists who are well-versed in the metabolic impacts of specific fatty acids. Best practices now include monitoring the duration of supplementation and avoiding long-term, high-dose regimens without periodic breaks or reassessments of blood lipid profiles. Applying this information in real-world scenarios requires a recognition that the benefits of a supplement are entirely dependent on the physiological context of the person taking it.
Redefining the Role of Supplements in Brain Repair
The discovery that certain components of fish oil could potentially impede the brain’s vascular repair mechanisms represented a significant shift in nutritional science. The findings demonstrated that while omega-3s remained essential nutrients, their application in the aftermath of neurological trauma was far more complex than previously understood. The analysis suggested that the focus must move from general supplementation to targeted, evidence-based lipid management.
Researchers concluded that the interaction between EPA and the cerebrovascular system created a unique vulnerability that prioritized anti-inflammatory signals over the structural needs of angiogenesis. Moving forward, the industry must emphasize the importance of precision and specificity in brain health protocols. The primary takeaway was a call for caution; the path to true cognitive resilience was found not in universal high-dose consumption, but in a deeper respect for the brain’s delicate and sophisticated healing processes. Professionals were urged to consider the timing and composition of fats to ensure that the recovery environment supported, rather than hindered, the restoration of the neural vascular network.